A kidney cancer diagnosis can usher in a period of profound uncertainty, fear, and a cascade of urgent questions for patients and their loved ones. However, amidst these challenges, a transformative shift in therapeutic approaches, particularly the advent of immunotherapy, is redefining the landscape of kidney cancer care, offering renewed hope and empowering individuals to make informed treatment decisions. This article explores the intricacies of kidney cancer, the revolutionary impact of immunotherapy, ongoing research, and the resources available to those navigating this journey.
Understanding Kidney Cancer: A Growing Health Challenge
Kidney cancer, medically known as renal cell carcinoma (RCC) in its most common form, develops when cells within the kidneys begin to grow uncontrollably, eventually forming a tumor. The kidneys, a pair of bean-shaped organs situated on either side of the spine, beneath the rib cage, are vital to maintaining bodily health. Each approximately the size of a fist, these organs perform several essential functions: filtering waste products from the blood, producing urine, regulating blood pressure, and supporting red blood cell production. Any disruption to their normal cellular function can have significant health implications.
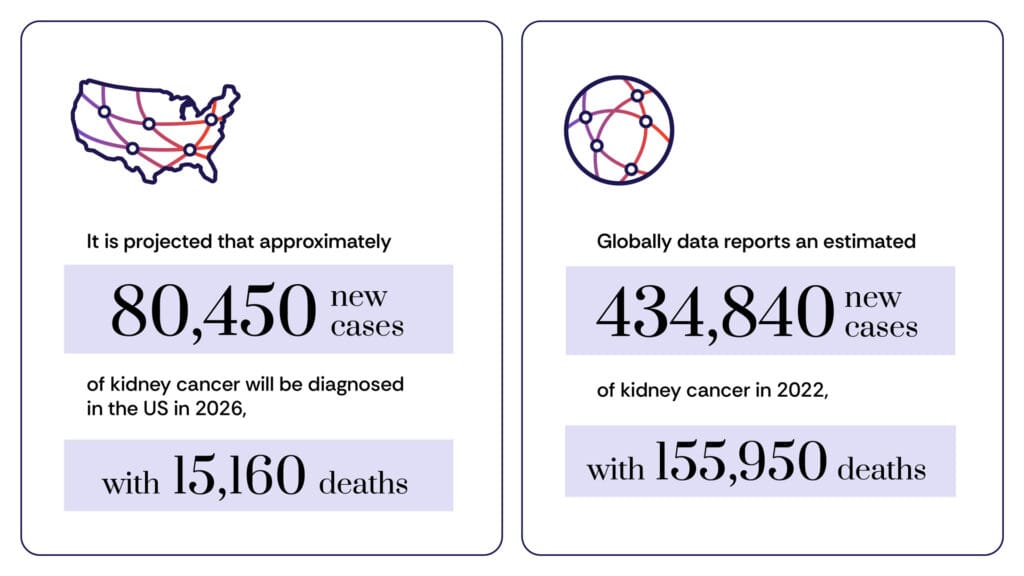
Kidney cancer represents a significant public health concern. It is consistently ranked among the top ten most common cancers in the United States, accounting for an estimated 3% to 5% of all cancer diagnoses. In 2023, the American Cancer Society projected approximately 81,880 new cases of kidney cancer and 14,890 deaths from the disease in the U.S. alone, highlighting its substantial impact. Globally, the incidence varies, but the trend of rising diagnoses has been observed in many developed nations. The disease typically affects older individuals, with the average age at diagnosis being 65. Furthermore, men are diagnosed with kidney cancer at nearly twice the rate of women, a disparity that researchers continue to investigate, potentially linking it to a combination of genetic, environmental, and lifestyle factors.
While several subtypes of kidney cancer exist, clear cell renal cell carcinoma (ccRCC) is by far the most prevalent, accounting for 75-80% of all cases. Other less common subtypes include papillary renal cell carcinoma (pRCC), chromophobe renal cell carcinoma, and collecting duct carcinoma, each with distinct pathological features and varying responses to treatment. Understanding the specific subtype is crucial for tailoring the most effective therapeutic strategy.
Risk factors for kidney cancer include smoking, obesity, hypertension, certain genetic conditions (such as von Hippel-Lindau disease), and long-term dialysis. Early-stage kidney cancer often presents without symptoms, leading to incidental diagnosis during imaging for other conditions. When symptoms do occur, they can include blood in the urine (hematuria), a lump in the abdomen, persistent back or side pain, fatigue, and unexplained weight loss.

The Immune System’s Role and the Rise of Immunotherapy
For decades, the primary arsenal against cancer relied on surgery, radiation, and chemotherapy. While effective for many, these treatments often came with significant side effects and limitations, particularly for advanced or metastatic disease. The late 20th and early 21st centuries witnessed a paradigm shift with the emergence of targeted therapies, which specifically attack cancer cells based on their molecular characteristics. However, the most profound revolution in recent memory has been the advent of immunotherapy.
Immunotherapy represents a fundamentally different approach to cancer treatment. Instead of directly attacking cancer cells, it harnesses the body’s own immune system to recognize, target, and eliminate cancer. The immune system is a complex network of cells, tissues, and organs that work together to protect the body from foreign invaders like bacteria, viruses, and abnormal cells, including cancer cells. Normally, immune cells, particularly T cells, are adept at identifying and destroying malignant cells. However, cancer cells are often cunning adversaries; they evolve mechanisms to evade immune surveillance. Some cancers can express proteins that act as "checkpoints," essentially sending "off" signals to T cells, thereby shutting down the immune response and allowing the tumor to grow unchecked.
Immunotherapy, particularly immune checkpoint inhibitors (ICIs), works by blocking these inhibitory signals. By releasing the "brakes" on the immune system, ICIs empower T cells to recognize and attack cancer cells more effectively. This innovative approach not only aims to eliminate existing cancer but, in some cases, can also establish a long-lasting immune memory, potentially reducing the chance of cancer recurrence.
A Paradigm Shift: Immunotherapy in Kidney Cancer Treatment
The integration of immunotherapy has dramatically altered the prognosis for many kidney cancer patients, particularly those with advanced or metastatic disease. Before immunotherapy, treatment options for metastatic RCC were limited, and prognosis was often poor. The introduction of vascular endothelial growth factor (VEGF) pathway inhibitors improved outcomes, but responses were often not durable. Immunotherapy, specifically immune checkpoint inhibitors, has changed this trajectory.
The core of current immunotherapy for kidney cancer lies in the use of ICIs that target the PD-1/PD-L1 pathway and the CTLA-4 pathway.
- PD-1 (Programmed cell death protein 1) inhibitors: These drugs block the PD-1 receptor on T cells, preventing it from binding to PD-L1 (Programmed death-ligand 1) on cancer cells. This effectively removes the "off" switch that cancer cells use to suppress T cell activity. Key FDA-approved PD-1 inhibitors for kidney cancer include Nivolumab (Opdivo) and Pembrolizumab (Keytruda).
- CTLA-4 (Cytotoxic T-Lymphocyte-Associated protein 4) inhibitors: These drugs block CTLA-4, another checkpoint receptor on T cells that acts as an early "brake" on T cell activation. Ipilimumab (Yervoy) is the primary CTLA-4 inhibitor used in kidney cancer.
Often, these inhibitors are used in combination to achieve a synergistic effect, unleashing a more potent anti-tumor immune response. For instance, the combination of Nivolumab (anti-PD-1) and Ipilimumab (anti-CTLA-4) has shown remarkable efficacy in intermediate- and poor-risk metastatic RCC. Similarly, combinations of PD-1 inhibitors with VEGF-targeted therapies (e.g., Pembrolizumab plus Axitinib or Lenvatinib, Nivolumab plus Cabozantinib, Avelumab plus Axitinib) have become standard first-line treatments for many patients, demonstrating superior outcomes compared to targeted therapy alone.

Milestones in Treatment: A Timeline of Progress
The journey of immunotherapy in kidney cancer has been marked by several significant milestones:
- 2015: Nivolumab (Opdivo), a PD-1 inhibitor, received its initial FDA approval for advanced renal cell carcinoma following prior anti-angiogenic therapy. This was a pivotal moment, introducing immunotherapy as a viable option for a challenging patient population.
- 2016: Nivolumab was also approved for use in combination with Ipilimumab (Yervoy), a CTLA-4 inhibitor, for intermediate- or poor-risk advanced RCC, based on the groundbreaking CheckMate 214 trial. This combination demonstrated superior overall survival compared to standard sunitinib.
- 2018-2019: The landscape expanded further with the approval of combination therapies involving PD-1 inhibitors and VEGF-targeted therapies. Key approvals included Avelumab (Bavencio) plus Axitinib (Inlyta), and Pembrolizumab (Keytruda) plus Axitinib, both for first-line treatment of advanced RCC, based on trials like JAVELIN Renal 101 and KEYNOTE-426, respectively. These combinations offered new, highly effective first-line options for a broader range of patients.
- Ongoing: Subsequent years have seen continued refinement of these strategies, with new combinations like Nivolumab plus Cabozantinib (Cabometyx) and Pembrolizumab plus Lenvatinib (Lenvima) further expanding the therapeutic arsenal and providing more tailored approaches based on patient risk stratification and disease characteristics.
These approvals represent a rapid evolution, moving from limited second-line options to potent first-line combinations that have fundamentally improved patient prognosis.
Efficacy and Hope: Data Driving the Revolution
The impact of immunotherapy on kidney cancer survival statistics has been profound. While the annual rate of new kidney cancer diagnoses has been rising for years, a truly encouraging trend is the concurrent fall in death rates. This positive divergence is a direct reflection of advances in treatment and care, with immunotherapy playing a central role in helping more people live longer and with a better quality of life.
Clinical trials have consistently demonstrated the superior efficacy of immunotherapy, either alone or in combination, compared to older treatments. For instance, studies have shown that for patients with intermediate- or poor-risk metastatic RCC, combination immunotherapy (e.g., nivolumab + ipilimumab) can achieve significantly higher objective response rates (ORR) and improved overall survival (OS) compared to VEGF-targeted therapies. Similarly, combinations of PD-1 inhibitors with VEGF inhibitors have shown marked improvements in progression-free survival (PFS) and OS across various patient populations, establishing new standards of care.
A hallmark of immunotherapy is the potential for durable responses and long-term remission in a subset of patients. Unlike conventional chemotherapy, which often sees responses wane over time, some patients treated with immunotherapy can experience sustained disease control for many years, even after discontinuing treatment. This durability offers a profound sense of hope and a paradigm shift in what is achievable for advanced kidney cancer.
Navigating the Landscape: Patient Empowerment and Clinical Decisions
Facing a kidney cancer diagnosis, whether personally or as a loved one, can feel overwhelmingly complex. The availability of advanced therapies like immunotherapy underscores the critical importance of becoming an empowered advocate for one’s own health. This involves educating oneself about the specific cancer type, understanding the array of treatment options available, and staying informed about ongoing research.
Central to this empowerment is open and thorough communication with the healthcare team. Immunotherapy is not a universal solution, and its suitability depends on numerous factors, including the specific cancer subtype, stage, prior therapies received, overall health status, and individual patient characteristics. It is imperative to engage in detailed discussions with oncologists to determine if immunotherapy is the right path.
Key questions patients should consider asking their care team about immunotherapy include:
- Is immunotherapy a suitable treatment option for my specific type and stage of kidney cancer?
- What are the specific immunotherapy drugs or combinations recommended, and why?
- What are the potential benefits and expected outcomes of immunotherapy for my condition, including response rates and survival data?
- What are the potential side effects of immunotherapy, and how will they be managed? How do these differ from chemotherapy side effects?
- How long will treatment last, and what is the administration schedule?
- What monitoring will be involved during and after treatment?
- Are there any clinical trials for kidney cancer immunotherapy that I might be eligible for?
- What are the financial implications and insurance coverage for immunotherapy?
- How will immunotherapy impact my daily life and quality of life?
Understanding these aspects allows patients to weigh the benefits and risks comprehensively, aligning treatment choices with their personal values and goals.
The Road Ahead: Cutting-Edge Research and Future Therapies
The rapid progress in kidney cancer treatment through immunotherapy is a testament to tireless research efforts, and the field continues to evolve at an astonishing pace. Current research is intensely focused on several critical areas:
- Improving Survival in Metastatic Cases: While current immunotherapies have transformed outcomes, not all patients respond, and many eventually develop resistance. Researchers are exploring novel combination strategies, including combining ICIs with other immunotherapies, targeted agents, or even conventional treatments, to enhance response rates and overcome resistance mechanisms.
- Reducing Recurrence After Surgery: For patients who undergo surgery for localized kidney cancer, there remains a risk of recurrence. Adjuvant immunotherapy (given after primary treatment) is being investigated to reduce this risk, with some agents already showing promise in extending disease-free survival.
- Personalized Vaccines and Biomarkers: A significant area of focus is personalized medicine. This includes developing cancer vaccines tailored to an individual’s tumor mutations, aiming to train the immune system to recognize and attack specific cancer cells. Furthermore, identifying reliable biomarkers (e.g., genetic mutations, protein expression levels) that can predict which patients are most likely to respond to specific immunotherapies is crucial for guiding treatment decisions and avoiding ineffective therapies.
- Novel Immunotherapies: Beyond checkpoint inhibitors, new classes of immunotherapies are under development. These include:
- CAR T-cell therapy: While primarily established for certain blood cancers, researchers are exploring its potential in solid tumors like kidney cancer, though significant hurdles remain.
- Oncolytic viruses: Viruses engineered to selectively infect and destroy cancer cells while also stimulating an immune response.
- Bispecific antibodies: Molecules designed to simultaneously bind to cancer cells and immune cells, bringing them into close proximity to facilitate tumor killing.
- Antibody-Drug Conjugates (ADCs): These combine the targeting specificity of antibodies with potent cytotoxic drugs, delivering chemotherapy directly to cancer cells.
- Cytokine therapies and cellular therapies: Further exploration of approaches that enhance the overall immune response against cancer.
This continued work is not merely adding to a list of treatment options; it is grounded in patient voices, shaping research priorities to address unmet needs. The future of kidney cancer treatment aims to deliver more effective, less toxic, and highly personalized therapies, giving every patient greater hope and more precious time.
Addressing Challenges and Ensuring Access
Despite the revolutionary advancements, challenges remain in the widespread implementation and optimization of immunotherapy for kidney cancer. The cost of these advanced therapies can be substantial, posing concerns about accessibility and equity, particularly in healthcare systems with varying coverage policies. Efforts are needed to ensure that all eligible patients, regardless of socioeconomic status or geographic location, can access these life-changing treatments.

Furthermore, while immunotherapy often has a different side effect profile than chemotherapy, it is not without its own set of potential adverse events. Immune-related adverse events (irAEs) can occur when the unleashed immune system mistakenly attacks healthy tissues, leading to inflammation in various organs (e.g., colitis, hepatitis, pneumonitis, endocrinopathies). Managing these irAEs requires specialized expertise and close monitoring, highlighting the need for trained oncology teams and robust supportive care protocols.
The complexity of choosing the optimal immunotherapy regimen, especially in combination with other agents, also necessitates ongoing education for healthcare providers. Understanding patient stratification, biomarker utility, and effective management of side effects is paramount to maximizing therapeutic benefit and minimizing harm.
Conclusion: A Future Illuminated by Research and Collaboration
The journey through a kidney cancer diagnosis is undoubtedly challenging, but the progress in immunotherapy offers a powerful beacon of hope. By empowering the body’s natural defenses, these treatments have transformed prognosis, extended lives, and improved the quality of life for countless patients. The continuous evolution of research, driven by dedicated scientists and clinicians worldwide, promises even more refined and effective therapies in the years to come.
As the scientific community delves deeper into the intricacies of the immune system and cancer biology, the future of kidney cancer treatment appears brighter than ever. For patients and their families, staying informed, advocating for personalized care, and seeking support from patient organizations and healthcare teams are crucial steps in navigating this evolving landscape. With ongoing collaboration between researchers, clinicians, and patients, the goal of achieving durable remission and a cure for kidney cancer moves ever closer.

