A New Era of Survival: The Numbers Behind the Breakthroughs
In a significant milestone for public health, the United States has achieved a historic five-year relative survival rate of 70% for all cancers combined during the period of 2015-2021. This figure represents a dramatic improvement from the mid-1970s, when the survival rate stood at a mere 49%. This nearly 50% increase in survival over approximately five decades is a powerful indicator of the impact of scientific progress, early detection initiatives, and more effective therapeutic strategies.
The most striking gains are observed in advanced, metastatic cancers, which were historically deemed untreatable just a generation ago. For conditions like metastatic melanoma, once associated with a grim prognosis, the landscape has fundamentally shifted. The report specifically highlights how survival for metastatic melanoma has improved from a sobering 16% to 35% in just 25 years. This transformation is largely attributed to the advent of groundbreaking treatments, notably immunotherapy and targeted therapies, which have revolutionized oncology. These are not incremental adjustments but represent a profound redefinition of what is achievable for patients facing the most aggressive forms of the disease.
The American Cancer Society, a leading voluntary health organization dedicated to eliminating cancer, has been publishing its Cancer Statistics reports annually for decades. These reports are considered definitive statistical summaries, drawing on data from sources like the National Cancer Institute (NCI), the Centers for Disease Control and Prevention (CDC), and state cancer registries. They provide crucial insights into cancer incidence, mortality, and survival trends across the U.S., guiding research priorities, public health policy, and clinical practice. The 2026 edition, therefore, builds upon a rich legacy of data collection and analysis, offering a detailed snapshot of the nation’s progress and ongoing struggles in the battle against cancer.
The Engine of Progress: Immunotherapy and Precision Medicine

The dramatic improvements in survival curves, especially for advanced cancers, are directly linked to the burgeoning fields of immunotherapy and targeted therapies. Immunotherapy, a revolutionary approach, harnesses the body’s own immune system to recognize and destroy cancer cells. This differs fundamentally from traditional treatments like chemotherapy, which directly attack cancer cells, or radiation, which damages them. Instead, immunotherapies, particularly immune checkpoint inhibitors, "release the brakes" on the immune system, allowing T-cells to mount a more robust and sustained attack against tumors.
Key examples of these breakthroughs include anti-PD-1 and anti-CTLA-4 therapies. Programmed death-1 (PD-1) and Cytotoxic T-Lymphocyte-Associated protein 4 (CTLA-4) are checkpoints that normally regulate immune responses to prevent autoimmune disease. Cancer cells often exploit these checkpoints to evade immune detection. Immune checkpoint inhibitors block these pathways, reactivating the immune system’s anti-tumor activity.
Dr. Antoni Ribas, MD, PhD, a Professor at UCLA and a member of the Cancer Research Institute (CRI) Scientific Advisory Council, emphasized this profound impact: "When we look at metastatic melanoma survival improving from 16% to 35% in just 25 years, we’re witnessing the direct impact of immune checkpoint inhibitors like anti-PD-1 and anti-CTLA-4 therapies. These are the breakthroughs that the Cancer Research Institute has championed for decades – supporting the fundamental science that made immunotherapies a reality." His statement underscores the critical role of sustained, long-term investment in basic scientific research, often spanning decades, which ultimately translates into life-saving clinical applications. Organizations like CRI and the National Cancer Institute have been instrumental in funding the foundational immunology research that paved the way for these therapeutic revolutions.
Targeted therapies, another pillar of modern cancer treatment, work by identifying and attacking specific molecular targets on cancer cells, often genes or proteins that contribute to cancer growth and spread. Unlike conventional chemotherapy, which can damage healthy cells along with cancerous ones, targeted therapies are designed to be more precise, leading to fewer side effects and improved efficacy for patients whose tumors possess these specific targets. The rise of genomic sequencing and personalized medicine has fueled the development of these highly specific treatments, matching therapies to the unique genetic profile of a patient’s tumor.
The Enduring Burden: Cancer’s Toll in America
Despite the significant strides in survival, cancer remains a formidable public health challenge. The ACS report confirms that cancer is the second leading cause of death in the U.S. overall. However, its impact is even more pronounced within specific age demographics: it stands as the leading cause of death for men aged 60-79 and women aged 40-79. This highlights the substantial burden cancer places on individuals in their prime productive years and older adults.
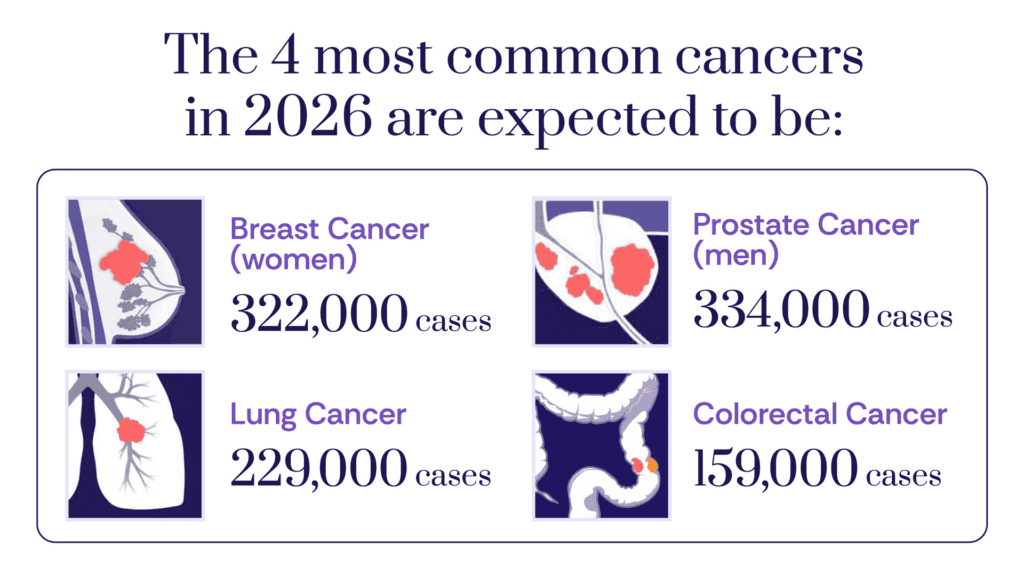
For 2026, the ACS estimates that approximately 2.1 million Americans will receive a cancer diagnosis, with an estimated 626,000 deaths. This translates to an average of about 5,800 new cases and 1,720 deaths every single day across the nation. These figures, while representing a declining overall mortality rate, underscore the sheer volume of individuals and families affected by the disease annually.
Among the various cancer types, lung cancer continues to be the deadliest, projected to cause more deaths than the second- and third-deadliest cancers—colorectal and pancreatic—combined. The high mortality rate of lung cancer is largely attributable to its often late diagnosis, aggressive nature, and challenges in effective early screening for all populations. Colorectal cancer, while benefiting from screening advancements, still contributes significantly to cancer mortality, as does pancreatic cancer, which remains one of the most challenging cancers to treat due to its rapid progression and resistance to many therapies.
Unpacking the Disparities: A Call for Equity
While the overall narrative of the Cancer Statistics 2026 report is one of progress, it concurrently shines a harsh light on the persistent and widening disparities in cancer care and outcomes. The cancer death rate has indeed declined by 34% from 1991 to 2023, translating to an estimated 4.8 million deaths averted. This broad progress is attributed to a combination of factors, including reduced smoking rates, enhanced early detection programs, and the advent of improved treatments, including the immunotherapy revolution. However, this progress has not been evenly distributed across all demographics and geographic regions.
The report identifies several critical areas where progress has been slower and where inequities are stark:
- Young Adults Face Rising Cancer Rates: A concerning trend highlighted in the report is the increasing incidence of certain cancers among young adults. This rise is observed in cancers such as colorectal cancer, often linked to lifestyle factors, dietary habits, and potentially environmental exposures. Additionally, cancers like uterine corpus cancer, which is also on the rise, are increasingly affecting younger populations, potentially driven by factors such as rising obesity rates and associated metabolic conditions. The reasons for these trends are complex and multifaceted, demanding further research into environmental, genetic, and lifestyle factors.
- Geographic Gaps Are Widening: Access to high-quality cancer care, including advanced diagnostics, specialized treatments, and clinical trials, often depends on where one lives. The report indicates widening geographic disparities, likely reflecting the uneven distribution of healthcare resources. Rural areas, for instance, often lack comprehensive cancer centers, oncologists, and advanced technology, forcing patients to travel long distances for care, which can be a significant barrier. Urban underserved communities may also face similar challenges due to socioeconomic factors and overwhelmed healthcare systems. These gaps exacerbate existing health inequities and result in poorer outcomes for those in underserved regions.
- Racial and Ethnic Inequities Persist – Driven by Systemic Barriers: Perhaps the most profound disparities highlighted in the report are those based on race and ethnicity. These inequities are not merely statistical but are deeply rooted in systemic barriers that permeate the healthcare system and society at large. The report explicitly emphasizes that these disparities stem from a "higher prevalence of risk factors, medical mistrust, and lack of insurance, which hinders access to high-quality health care." For instance, Black women continue to face higher mortality rates from breast cancer despite similar incidence rates to white women, largely due to later diagnoses and less access to optimal treatment. Similarly, Black men experience higher incidence and mortality rates from prostate cancer.
Even after accounting for factors like stage at diagnosis and socioeconomic status, survival gaps remain. The report identifies "less access to high-quality care across the cancer continuum, from prevention to diagnosis and treatment" as the "largest contributor" to these persistent disparities. This encompasses everything from inadequate screening uptake due to lack of awareness or access, to delays in diagnosis, to receiving suboptimal or delayed treatment, and insufficient access to palliative and supportive care. These systemic issues demand comprehensive policy changes and targeted community-based interventions to foster trust and ensure equitable access to care for all populations.
The Road Ahead: Persistent Challenges and Future Horizons

The Cancer Statistics 2026 report serves as a powerful validation of the immense value of sustained research. The immunotherapy revolution, with its profound impact on patient survival, did not materialize overnight. It was meticulously built upon decades of foundational basic science, generously funded by institutions like the National Cancer Institute and philanthropic organizations such as the Cancer Research Institute. This long-term investment in understanding the fundamental biology of cancer and the immune system has undeniably yielded a remarkable return.
However, the same data that celebrates these monumental advancements also starkly reveals how much work remains. Not all cancers have seen similar breakthroughs. Pancreatic cancer, for example, remains a formidable challenge, with its five-year survival rate stubbornly stagnant at just 13%. This means that an estimated 185 Americans diagnosed with pancreatic cancer today face essentially unchanged odds compared to those diagnosed decades ago. The aggressive nature of the disease, coupled with late-stage diagnoses due to a lack of early symptoms and effective screening methods, contributes to its devastating prognosis.
Similarly, uterine corpus cancer mortality continues its alarming 26-year climb. This rise is particularly concerning given its potential links to increasing rates of obesity and metabolic syndrome, highlighting the complex interplay between lifestyle, public health, and cancer outcomes. These stagnant or worsening trends for specific cancer types underscore the urgent need for dedicated research funding, innovative diagnostic tools, and novel therapeutic strategies tailored to these resistant diseases.
The implications of the Cancer Statistics 2026 report extend beyond the scientific community, touching upon public health policy, healthcare access, and social equity. The findings present a clear mandate: every patient, regardless of their background or geographic location, deserves access to the latest advances in cancer care, including cutting-edge immunotherapies and targeted treatments. Every cancer type, including those with historically poor prognoses like pancreatic and uterine cancers, warrants intensified research investment to unlock new breakthroughs. And fundamentally, every community—irrespective of race, ethnicity, or socioeconomic status—deserves equal access to life-saving cancer prevention, diagnosis, and treatment.
The immune system holds extraordinary, untapped power to fight cancer. Continued, robust investment in cancer immunology research, alongside concerted efforts to dismantle systemic barriers to care, is essential to fully unlock that power and extend its promise of hope and extended life to patients everywhere. The journey is far from over, but the path forward is illuminated by both remarkable triumphs and critical challenges, demanding a collective, unwavering commitment to a future free from the burden of cancer.

