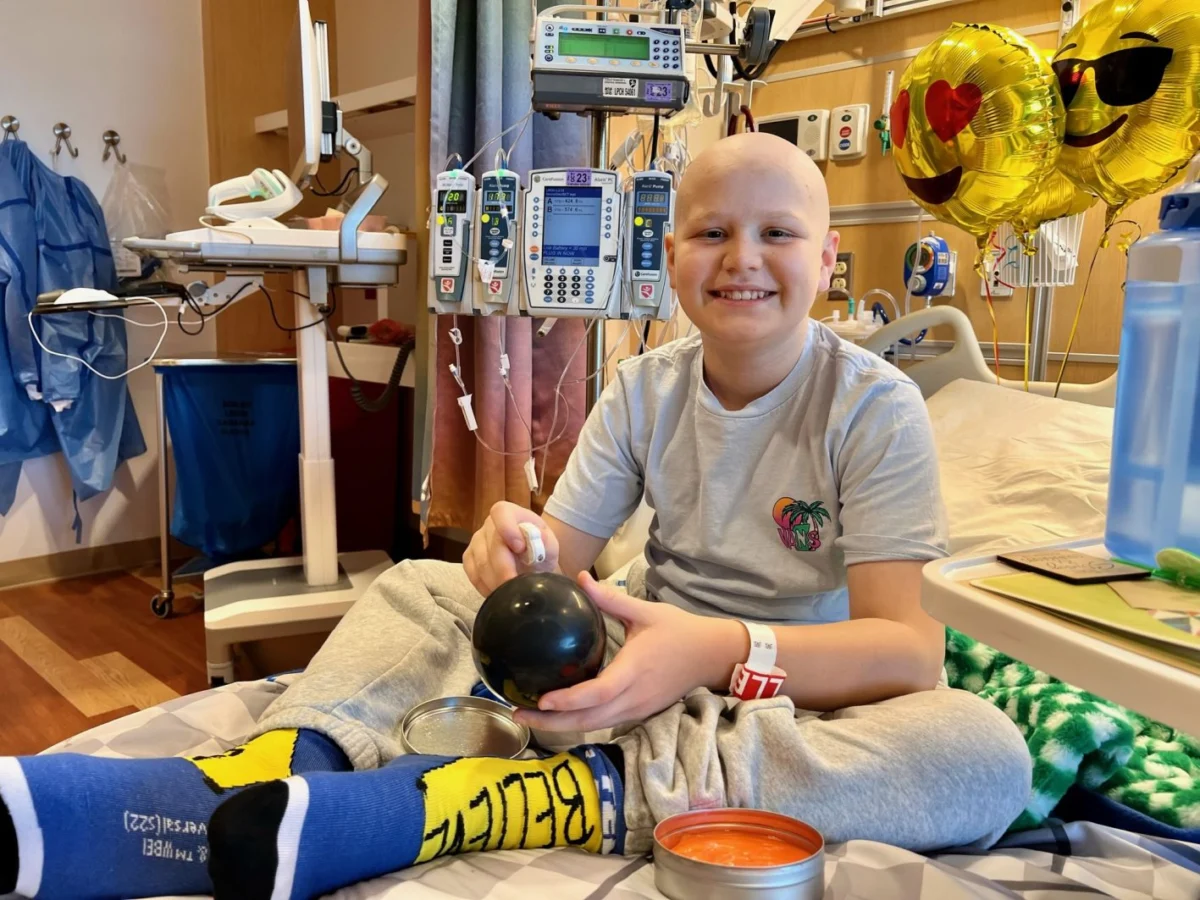
The diagnostic journey for pediatric cancer often begins with ambiguous symptoms that can mimic common childhood ailments, leading to critical delays in treatment. In the case of Max, a teenager living with Type 1 diabetes, a persistent abdominal pain was repeatedly dismissed by medical professionals as simple constipation. Over a period of three weeks and three separate visits to the emergency department, his mother, Paige, found herself in the role of a primary medical advocate, challenging the clinical consensus that the issue would "work itself out" through increased fiber intake and hydration. This persistence ultimately led to an MRI that revealed a far more sinister reality: a large tumor caused by Burkitt lymphoma, an exceptionally aggressive form of non-Hodgkin lymphoma. The transition from a diagnosis of gastrointestinal distress to a life-threatening malignancy highlights the complexities of pediatric diagnostics and the vital importance of parental intuition in the clinical setting.
The Diagnostic Threshold and Burkitt Lymphoma
Burkitt lymphoma is recognized in the medical community as one of the fastest-growing human tumors. It is a high-grade B-cell neoplasm characterized by the translocation of the MYC gene, which leads to the rapid and uncontrolled proliferation of lymphocytes. Because the tumor cells can double in mass within 24 to 48 hours, any delay in diagnosis can significantly alter the patient’s prognosis. For Max, the three-week delay represented a period of immense risk.
When the MRI finally confirmed the presence of a mass, the medical team’s focus shifted instantly from conservative management to intensive intervention. Burkitt lymphoma, while highly aggressive, is also notably sensitive to chemotherapy. The very metabolic activity that makes the cancer dangerous—its rapid division—also makes it vulnerable to cytotoxic agents that target dividing cells. Doctors informed the family that while the diagnosis was severe, the "lack of resilience" in the cancer cells offered a high probability of successful treatment if the protocol was followed rigorously.
The Chronology of Treatment and Medical Complexity
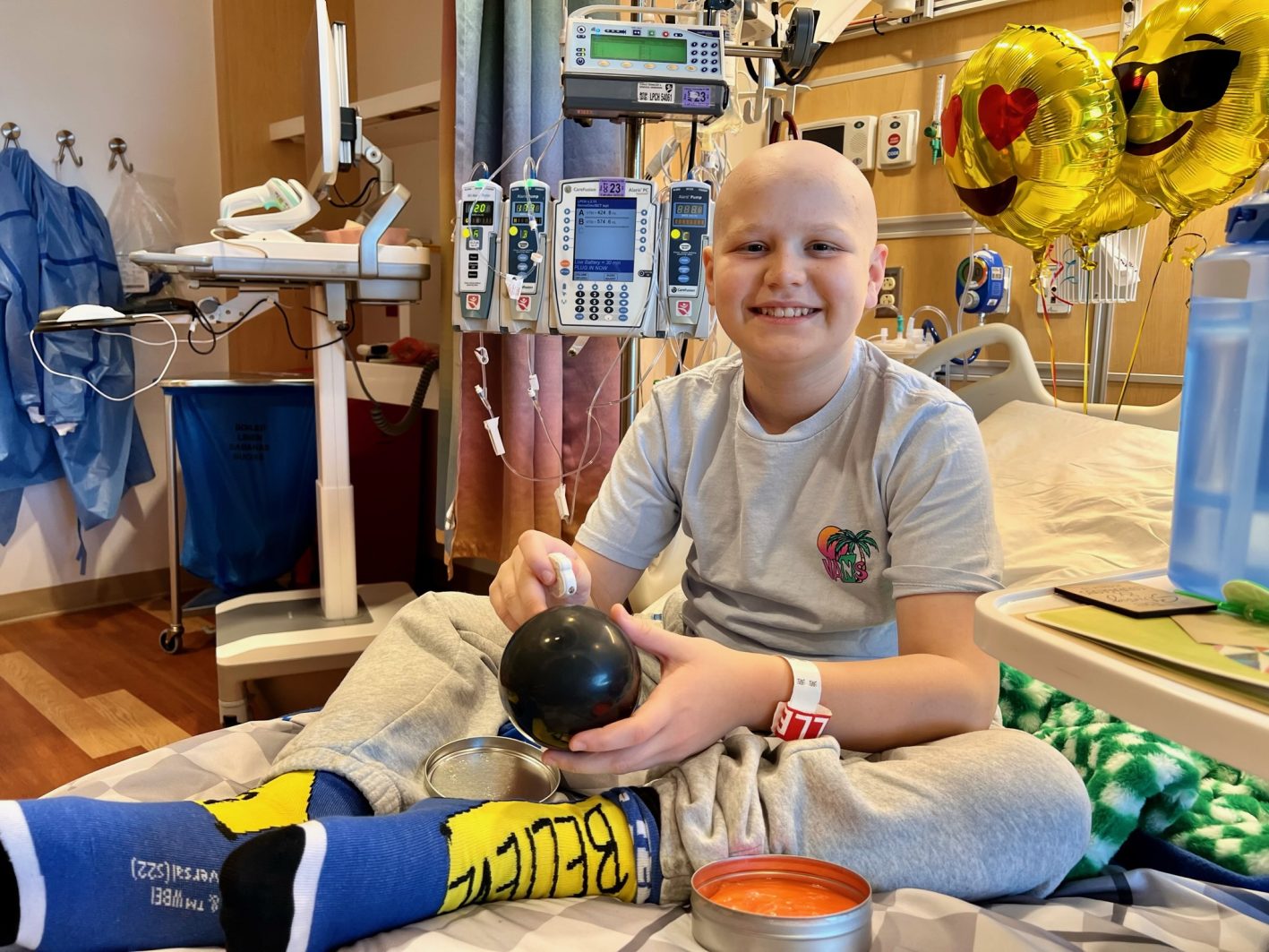
Max’s treatment plan was comprehensive and immediate, requiring a bone marrow biopsy, multiple lumbar punctures to check for central nervous system involvement, the surgical placement of a chemo-port, and the initiation of high-dose chemotherapy. What would have been a grueling regimen for any patient was further complicated by Max’s pre-existing Type 1 diabetes (T1D).
The management of T1D during oncology treatment presents a unique set of clinical hurdles. Chemotherapy often induces nausea and alters appetite, making it difficult to predict carbohydrate intake. Furthermore, the standard use of corticosteroids (such as prednisone or dexamethasone) to mitigate the side effects of chemotherapy or to assist in the destruction of lymphoma cells causes a massive spike in blood glucose levels. For a patient like Max, who uses a continuous glucose monitor (CGM) and an insulin pump, the "steroid storm" meant his insulin requirements fluctuated wildly.
A significant logistical issue emerged during his inpatient stays: the hospital’s electronic health record (EHR) system lacked the capability to integrate real-time data from his CGM. This forced his parents to manually record carbohydrates, blood glucose readings, and insulin doses on paper for nurses to enter into the system later. This technological gap added an immense layer of "caregiver burden" to an already stressful situation, highlighting a need for better integration of wearable health technology within hospital infrastructures.
Psychological Resilience and Coping Mechanisms
The psychological impact of a cancer diagnosis on a teenager is profound. Max’s initial reaction was the fear of mortality, a common response to a disease often associated with death in popular media. However, once the "treatability" of the cancer was explained, he shifted his focus toward a personal goal: outlasting the disease’s own lack of resilience.
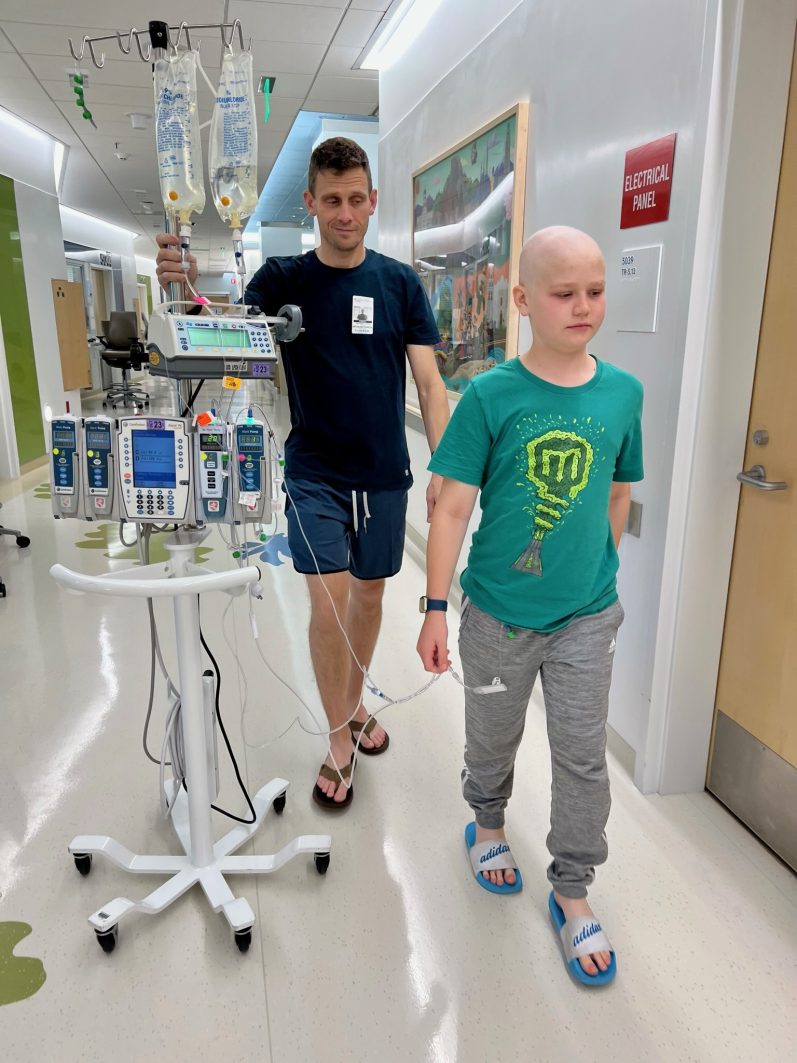
Max’s approach to his treatment was marked by a desire for autonomy. In pediatric oncology, younger children are typically sedated for invasive procedures like lumbar punctures—where a needle is inserted into the spinal canal to deliver chemotherapy or withdraw fluid. Max, however, chose to remain awake for these procedures. The loss of control associated with general anesthesia was, for him, more distressing than the procedure itself.
To combat the physical toll of the hospital environment, Max utilized modern technology in unconventional ways. He used a Meta Quest virtual reality headset to play "Gorilla Tag," a high-intensity game that required significant upper-body movement. This served as a form of "gamified physical therapy," helping him maintain muscle tone and cardiovascular health during weeks of confinement. His father, Zac, noted that these efforts were essential for staving off the muscle atrophy that frequently accompanies long-term hospitalization.
The Physical and Sensory Toll of Imaging
While chemotherapy and surgery are often viewed as the primary challenges of cancer, the diagnostic and monitoring phases can be equally taxing. Max’s experience with PET (Positron Emission Tomography) and CT (Computed Tomography) scans illustrates the sensory overload and physical discipline required of pediatric patients.
A PET/CT scan requires the patient to lie perfectly still for extended periods—sometimes up to three hours—inside a narrow, loud, and often hot tube. For Max, the experience was compounded by the requirements of his diabetes management; if his blood sugar was not within a specific range at the time of the scan, the radioactive tracer used to identify cancer cells would not be absorbed correctly, potentially ruining the image. Zac described the environment inside the scanner as a "sensory prison," comparing the high-volume mechanical clanging to the introductory sequence of Pink Floyd’s song "Money." Max utilized visualization and rhythmic mantras—such as "this is not permanent"—to endure the claustrophobia and heat.
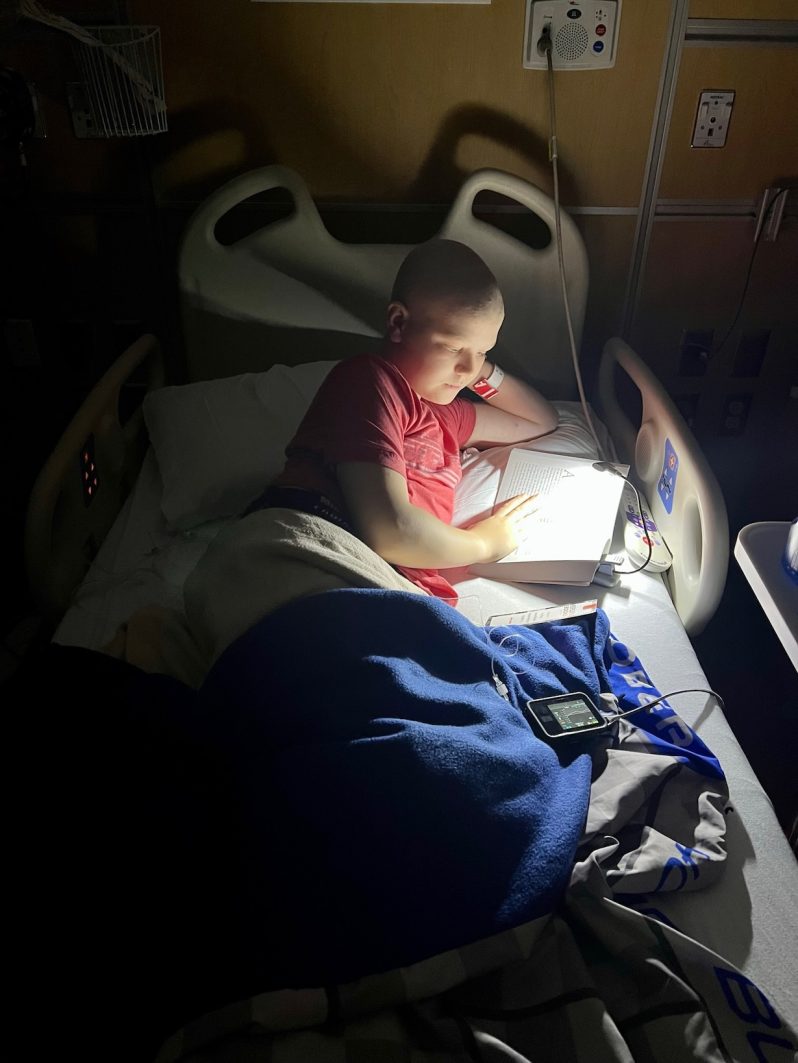
The Legacy of Clinical Trials and Research
The fact that Max is currently in remission and pursuing an active life is a testament to decades of clinical research. In the mid-20th century, Burkitt lymphoma was almost universally fatal. The current "gold standard" protocols were developed through rigorous clinical trials involving thousands of previous patients. These trials determined the precise combinations of cyclophosphamide, vincristine, doxorubicin, and methotrexate that maximize "kill rates" while managing toxicity.
Paige emphasized that her son’s survival is inextricably linked to the families who participated in research before them. This awareness has influenced Max’s own career aspirations. Now a high school freshman, he has expressed a desire to become a biologist focused on curing diseases. His goal is to contribute to the same body of scientific knowledge that provided him with a second chance at life.
Broader Implications for Pediatric Healthcare
Max’s story offers several critical insights for the broader medical community and the public:
- The Necessity of Parental Advocacy: The case underscores that parents are often the first to recognize subtle deviations in a child’s health. Healthcare systems must ensure there are clear pathways for "escalation of concern" when a parent feels a diagnosis is incomplete.
- Interdisciplinary Care for Comorbidities: As more children survive chronic illnesses like T1D, oncology wards must become more adept at managing these "dual-diagnosis" patients. The integration of specialized endocrinology support within oncology units is becoming a necessity rather than a luxury.
- Digital Health Integration: There is a pressing need for hospitals to upgrade their EHR systems to communicate with consumer medical devices. Manual data entry in an era of real-time cloud-based glucose monitoring is an inefficiency that increases the risk of medical errors.
- Holistic Recovery: Recovery from cancer is not merely the absence of disease but the restoration of a full life. Max’s transition from a hospital bed to rowing six days a week and participating in a Civil Air Patrol encampment in Germany demonstrates the importance of "looking forward" as a therapeutic tool.
Conclusion
Today, Max’s life is defined not by the "poop to cancer" transition of his diagnosis, but by his pursuit of rigorous physical and academic challenges. His participation in the Civil Air Patrol European Encampment—a program involving military drills, aerospace education, and leadership training—serves as a powerful coda to his period of physical vulnerability.

The success of his treatment is a victory for modern medicine, but the journey reveals the gaps that still exist in diagnostic speed and technological integration. For Paige and Zac, the milestones of a normal life—birthdays, the first day of high school, rowing competitions—carry a weight they never previously imagined. Max’s message to other children facing similar battles remains one of psychological fortitude: the belief that through positive visualization and a refusal to be outworked by the disease, one can find a path through the most aggressive of circumstances.