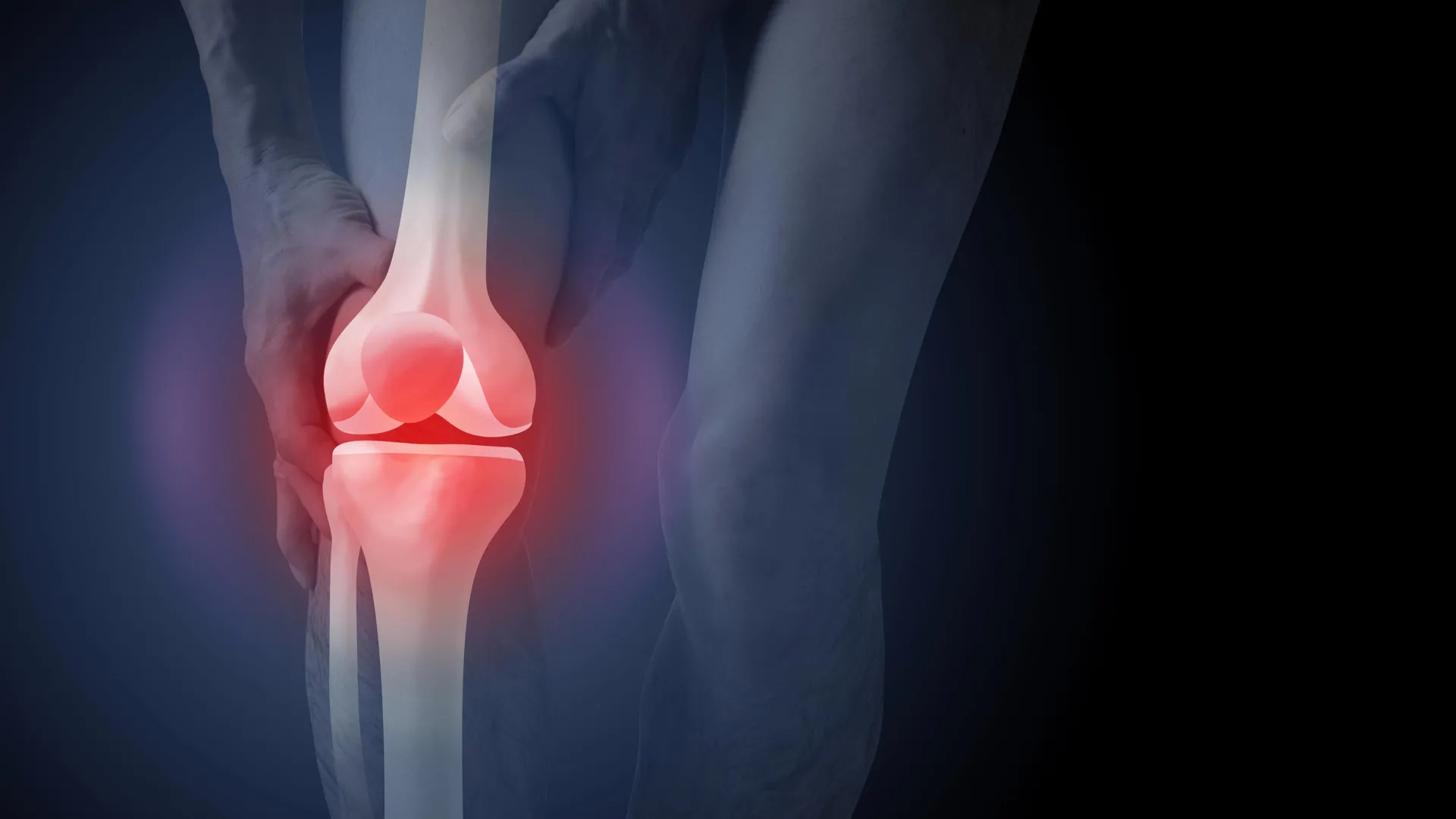
The traditional medical pathway for diagnosing knee pain is undergoing a significant reassessment as new research highlights the psychological and financial consequences of routine imaging. Despite national clinical guidelines advising against the use of X-rays for the initial diagnosis of knee osteoarthritis, nearly half of all patients in Australia presenting with knee pain are still referred for imaging. This practice not only costs the Australian healthcare system an estimated A$104.7 million annually in diagnostic fees but, according to a recent study published in PLOS Medicine, may also be actively harming patient outcomes by skewing perceptions of the disease and encouraging a premature reliance on invasive surgical interventions.
Knee osteoarthritis is a chronic condition characterized by changes within the joint, including the degradation of cartilage, bone remodeling, and inflammation of the surrounding ligaments and muscles. While it was long described as a simple "wear and tear" disease, modern medicine views it as a complex failure of the joint’s natural repair mechanisms. As the population ages and obesity rates rise, the prevalence of the condition has surged, placing an unprecedented burden on the public health system. In the 2020–21 financial year, hospital services related to osteoarthritis, primarily driven by joint replacement surgeries, cost the Australian government approximately $3.7 billion.
The Disconnect Between Imaging and Patient Reality
One of the most persistent myths in musculoskeletal medicine is that the severity of joint damage visible on an X-ray correlates directly with the level of pain a patient experiences. However, decades of clinical data suggest otherwise. Many individuals with significant structural changes visible on an X-ray report little to no pain, while others with "clean" scans suffer from debilitating symptoms.
Because of this weak correlation, the Australian Commission on Safety and Quality in Health Care, along with international bodies like the National Institute for Health and Care Excellence (NICE) in the UK, recommends a "clinical diagnosis." This approach relies on a patient’s medical history and physical symptoms rather than pictures. Specifically, guidelines state that a diagnosis can be confidently made if a patient is 45 years or older and experiences activity-related joint pain with either no morning stiffness or stiffness that lasts less than 30 minutes.
Despite these clear directives, the culture of "defensive medicine" and patient expectations continue to drive high rates of imaging. Patients often feel that their pain is not being taken seriously unless a scan is performed, and many General Practitioners (GPs) find it quicker to order a test than to explain why one is unnecessary.
Insights from the PLOS Medicine Study
To understand the psychological impact of this diagnostic habit, researchers conducted a comprehensive study involving 617 participants across Australia. The study utilized a randomized controlled trial design where participants were asked to engage with one of three hypothetical consultation scenarios regarding knee pain.
In the first group, the patient received a clinical diagnosis based solely on their age and symptoms. In the second group, an X-ray was used to confirm the diagnosis, but the patient was not shown the images. In the third group, the patient was given an X-ray-based diagnosis and was shown the actual radiographic images of their joint.
The results revealed a stark contrast in patient outlook based on the diagnostic method used. Participants who were shown their X-ray images reported a 36% higher perceived need for knee replacement surgery compared to those who received a clinical diagnosis. Furthermore, the "imaged" group expressed significantly higher levels of "kinesiophobia"—a fear of movement. They were more likely to believe that exercise and physical activity would cause further damage to their joints, and they expressed greater anxiety about the long-term prognosis of their condition.
Ironically, the study found that patients were slightly more satisfied with an X-ray-based diagnosis than a clinical one. This suggests a dangerous feedback loop: patients want the very tests that may ultimately lead them toward more fear, less activity, and unnecessary surgery.
The Financial and Physical Toll of Over-Imaging
The implications of over-imaging extend far beyond the $104.7 million spent on the scans themselves. When an X-ray leads a patient to believe their knee is "bone-on-bone"—a common but often inaccurate descriptor—the psychological shift toward surgery begins. In 2021–22, more than 53,000 Australians underwent knee replacement surgery for osteoarthritis.
While total knee arthroplasty is a highly effective procedure for those with end-stage disease who have exhausted all other options, it is not without risk. Major surgery carries the potential for serious adverse events, including deep vein thrombosis (blood clots), pulmonary embolisms, and surgical site infections. Furthermore, clinical studies indicate that up to 20% of patients who undergo knee replacement remain dissatisfied with their results or continue to experience chronic pain post-surgery.
By diverting patients toward surgery prematurely, the healthcare system misses the opportunity to implement high-value, low-risk treatments. The gold standard for managing knee osteoarthritis includes:
- Education: Helping patients understand that the joint is not "wearing out" but needs strengthening.
- Exercise: Targeted physical therapy to improve joint stability and muscle support.
- Weight Management: Reducing the mechanical load on the knee joints.
When these non-surgical interventions are prioritized, many patients find they can manage their symptoms effectively for years, or even decades, without ever needing to enter an operating theater.
A Chronology of Changing Standards
The shift away from routine imaging is part of a broader movement in global medicine known as "Choosing Wisely," which aims to reduce low-value care.
- Pre-2000s: Osteoarthritis was largely viewed through a mechanical lens. X-rays were considered the "gold standard" for diagnosis, and "wear and tear" was the primary metaphor used by clinicians.
- 2010s: Large-scale longitudinal studies began to prove the disconnect between imaging and pain. Organizations like the Australian Commission on Safety and Quality in Health Care began drafting new Clinical Care Standards.
- 2017–2020: The Australian Knee Osteoarthritis Clinical Care Standard was formalized, explicitly stating that X-rays should not be routine.
- 2024: The PLOS Medicine study provides the first robust evidence of how these diagnostic choices specifically alter patient psychology and surgical demand.
Broader Implications for Musculoskeletal Health
The phenomenon observed in knee osteoarthritis is not an isolated incident. Similar trends have been documented in the management of low back pain and shoulder impingement. In cases of back pain, for instance, patients who receive early MRI scans often have worse outcomes and higher rates of surgery than those who do not, primarily because the scans reveal "incidentalomas"—normal age-related changes that are misinterpreted as the source of pain.
The "labeling effect" of a medical scan can be profound. Once a patient sees a narrowed joint space or a bone spur on a screen, that image becomes their internal reality. It overrides the body’s actual functional capacity. This latest research suggests that the language health professionals use, and the diagnostic tools they reach for, are just as important as the treatments they prescribe.
The Path Forward for Patients and Practitioners
For the medical community, the challenge lies in de-implementing a deeply ingrained habit. Reducing unnecessary X-rays requires a shift in GP training and a commitment to longer consultations where the "why" of a clinical diagnosis can be explained.
For patients, the message is one of empowerment. A diagnosis of knee osteoarthritis is not a sentence for future disability or an inevitable appointment with a surgeon. By focusing on movement, strength, and weight management, most individuals can maintain an active lifestyle.
Experts suggest that if a healthcare provider recommends an X-ray for knee pain without signs of acute trauma (such as a fall or inability to bear weight), patients should feel comfortable asking how the results of that scan will change their treatment plan. If the answer is that the treatment—exercise and weight management—remains the same regardless of the image, the scan may be more of a hindrance than a help.
Ultimately, the goal of modern osteoarthritis care is to treat the person, not the picture. By reducing the reliance on routine imaging, Australia can save millions in healthcare costs, reduce unnecessary radiation exposure, and, most importantly, prevent thousands of patients from falling into a cycle of fear and avoidable surgery.