The medical journey of Anikah Schmidt began with a series of subtle, seemingly innocuous symptoms that eventually unveiled a life-altering diagnosis. At 19 months old, a stage of development characterized by the physical milestones of walking and exploring, Anikah began to exhibit a noticeable loss of balance. While her parents, Vanessa and Ben, initially attributed the frequent stumbles to the typical clumsiness of a toddler, the emergence of a secondary symptom—persistent morning vomiting—signaled a deeper neurological crisis. This pattern of early-morning emesis is a classic clinical indicator of increased intracranial pressure, a red flag that often points toward serious central nervous system pathologies.
After a frustrating period of diagnostic uncertainty involving blood tests and dietary adjustments, a computed tomography (CT) scan provided the definitive and devastating answer. Anikah was diagnosed with an ependymoma, a primary central nervous system tumor that, in her case, had grown to the size of a golf ball. The mass was obstructing the flow of cerebrospinal fluid, necessitating immediate surgical intervention to relieve the life-threatening pressure on her brain. Within hours of the scan, the toddler was transitioned from a pediatrician’s office to an operating room, marking the beginning of a sixteen-year battle that highlights the complex reality of pediatric cancer: the "cure" often carries a lifelong price.
The Clinical Challenge of Ependymoma
Ependymomas are the third most common type of brain tumor in children, arising from the ependymal cells that line the ventricles of the brain and the center of the spinal cord. According to data from the Central Brain Tumor Registry of the United States (CBTRUS), these tumors represent about 6% to 10% of pediatric brain tumors. The primary treatment protocol typically involves maximal surgical resection followed by localized radiation. For Anikah, the initial surgery was deemed a success; her neurosurgeon reported a total gross resection, meaning the visible mass of the tumor had been entirely removed.

However, in the field of pediatric oncology, surgical removal is rarely the final step. To eliminate microscopic cancer cells that might remain, Anikah’s medical team recommended proton beam radiation. At the time of her diagnosis, this advanced form of treatment was not widely available, available only at a select few institutions across the United States. Proton therapy is often preferred for pediatric patients because it allows for more precise targeting of the tumor site, theoretically sparing the surrounding healthy brain tissue from the exit-dose radiation typical of traditional X-ray (photon) therapy. Seeking the best possible outcome, the Schmidt family relocated from their home in Minnesota to Houston, Texas, for an eight-week course of daily radiation at the MD Anderson Cancer Center.
The Paradox of Treatment-Induced Injury
The trajectory of Anikah’s recovery took a harrowing turn months after the family returned to Minnesota. Despite the successful removal of the tumor and the completion of radiation, her balance issues resurfaced with greater severity. She began to struggle with basic functions, including eating and swallowing, eventually leading to a catastrophic collapse where she ceased breathing. Medical imaging revealed that the very treatment intended to save her life—the proton radiation—had caused severe swelling and necrosis on her brain stem.
The brain stem is the most critical area of the central nervous system, controlling fundamental life functions such as heart rate, breathing, and consciousness. The radiation-induced inflammation in this delicate area placed Anikah in a state of neurological crisis. To survive, she required a tracheostomy, a ventilator to assist her breathing, and a feeding tube (G-tube) for nutrition. While hyperbaric oxygen therapy—a treatment that involves breathing pure oxygen in a pressurized environment—was eventually successful in arresting the swelling, the damage to her neurological pathways was permanent. This phenomenon, often referred to as "late effects" of cancer treatment, underscores a significant challenge in pediatric medicine: the developing brain of a toddler is exceptionally vulnerable to the high-energy particles used in cancer therapy.
A Chronology of Survivorship
The timeline of Anikah’s life since her diagnosis reflects the enduring nature of pediatric cancer survivorship. Her medical history is not categorized by a "pre-cancer" and "post-cancer" era, but rather a continuous management of treatment-related disabilities.
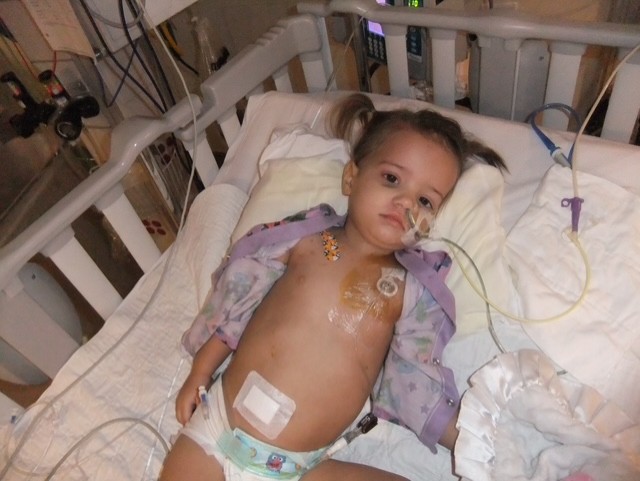
- 19 Months: Diagnosis of a golf-ball-sized ependymoma; emergency surgery for pressure relief; total tumor resection.
- Post-Surgery (Toddlerhood): Eight weeks of proton beam radiation in Houston.
- Post-Radiation Crisis: Development of brain stem swelling; respiratory failure; placement of tracheostomy, ventilator, and feeding tube.
- Early Childhood: Years of intensive physical, occupational, and speech therapy to regain basic motor functions and the ability to walk independently.
- Fourth Grade: Successful decannulation (removal of the tracheostomy tube), allowing for improved speech and social interaction.
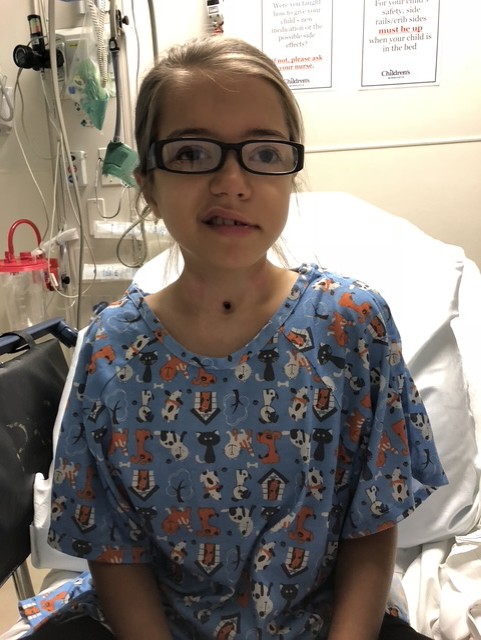
- Age 16 (Current): Ongoing reliance on a feeding tube for nutrition and supplemental oxygen during sleep; use of a walker in crowded environments for safety.
Now a teenager, Anikah’s life is a testament to resilience, yet it is also a reminder of the limitations imposed by her early medical trauma. While she participates in high school activities such as theater, cheerleading, and adapted dance, the physical toll of her history remains ever-present. The social milestones of adolescence, such as sleepovers or unassisted outings, are complicated by her need for nocturnal oxygen and specialized care.
The Broader Impact: Data on Pediatric Cancer Late Effects
Anikah’s story is not an isolated incident but a representative case of a growing population of childhood cancer survivors. Advances in medical technology have pushed the five-year survival rate for all childhood cancers to over 80%. However, this increase in survival has revealed a secondary epidemic of chronic health conditions.
Research published in the Journal of Clinical Oncology indicates that by the age of 50, approximately 99% of childhood cancer survivors will have developed at least one chronic health condition related to their previous treatment. Furthermore, nearly 80% will face a life-threatening or severe disability. These "late effects" can include:
- Neurological Impairments: Cognitive delays, balance issues, and hearing loss.
- Endocrine Disorders: Growth hormone deficiencies, thyroid issues, and infertility.
- Secondary Malignancies: A higher risk of developing new, unrelated cancers later in life due to previous radiation and chemotherapy exposure.
- Cardiovascular Disease: Damage to the heart and blood vessels caused by specific chemotherapy agents.
For families like the Schmidts, the financial and emotional burden is immense. The cost of lifelong physical therapy, medical equipment, and specialized educational support often exceeds the cost of the initial cancer treatment. Vanessa Schmidt’s observation—"We fixed the cancer—why can’t we fix everything else?"—encapsulates the frustration felt by many parents who find themselves navigating a healthcare system that is better equipped to treat acute illness than to manage chronic, treatment-induced disability.
The Role of Community and Psychosocial Support
Recognizing that medical intervention is only one facet of care, organizations like the Children’s Cancer Research Fund (CCRF) have pivoted toward supporting the holistic needs of survivors. One such initiative is Camp Norden, a specialized summer camp designed for children and teens affected by cancer.
For Anikah, attending Camp Norden represented a rare opportunity to exist in a space where her medical history was the norm rather than an anomaly. In a traditional school setting, her use of a walker or her feeding tube makes her a "kid with special needs." At Camp Norden, these are shared experiences. The psychological impact of such environments is profound; they offer survivors a sense of agency and belonging that is often stripped away in clinical settings. The anecdote of Anikah completing push-ups at camp—taking longer to position herself but finishing to the cheers of her peers—illustrates the importance of inclusive environments that prioritize ability over limitation.
Implications for Future Research and Policy
The case of Anikah Schmidt highlights the urgent need for a shift in pediatric oncology research. While the primary goal remains the eradication of the tumor, there is an increasing emphasis on "de-escalation" of treatment—finding ways to achieve high cure rates with lower doses of toxic radiation and chemotherapy.
- Precision Medicine: Developing targeted therapies that attack specific genetic mutations in tumors without harming healthy brain tissue.
- Neuro-regeneration: Researching ways to repair brain stem damage and other neurological injuries caused by radiation.
- Survivorship Clinics: Establishing more specialized clinics that provide multidisciplinary care for the long-term physical and mental health needs of survivors.
The narrative of "winning the war on cancer" is often simplified in public discourse to a binary of life or death. However, as Anikah’s sixteen-year journey demonstrates, survival is often the beginning of a new, complex chapter. True success in pediatric oncology must eventually be measured not just by the absence of disease, but by the quality of life afforded to those who survive it. Through continued research into less toxic treatments and robust support systems for survivors, the medical community aims to ensure that future patients can leave the shadow of cancer behind, rather than living within it for the rest of their lives.

