The diagnosis of a life-threatening illness in a toddler is a moment that fundamentally alters the trajectory of a family’s life, transforming ordinary milestones into profound victories. For two-year-old Emma and her parents, Ashley and Jacob, this reality began on a day that should have been marked by celebration: Emma’s second birthday. Instead of a traditional party, the family found themselves on the seventh floor of Children’s Minnesota, facing a diagnosis of acute myeloid leukemia (AML) with a RAM phenotype. This rare and aggressive form of leukemia carries a staggering 15% survival rate, a statistic that would daunt even the most resilient. However, through a combination of innovative medical research, compassionate use of experimental drugs, and a family philosophy centered on "celebrating everything," Emma’s story is becoming a testament to the evolving landscape of pediatric oncology.
The Path to Diagnosis: From Common Symptoms to the Seventh Floor
The onset of Emma’s illness was deceptive, manifesting as symptoms often associated with routine childhood ailments. Ashley and Jacob noticed their daughter, typically a high-energy child they described as "full-throttle," had become uncharacteristically lethargic and appeared to be in persistent discomfort. Initial medical consultations suggested a viral infection or a urinary tract infection. However, when standard antibiotic treatments failed to alleviate her pain or restore her energy, her parents sought emergency care at Children’s Minnesota.
The transition from the emergency room to the oncology ward was swift and jarring. Upon arrival, the medical team determined that Emma required specialized care. Ashley recalls the moment the elevator doors opened on the seventh floor, revealing the sign for "hematology/oncology." It was there that Emma was diagnosed with AML-RAM. Acute myeloid leukemia is a cancer of the blood and bone marrow characterized by the rapid growth of abnormal white blood cells. The RAM phenotype is a specific, high-risk genetic marker associated with poor prognosis and resistance to conventional chemotherapy.
On her second birthday, Emma began her first round of chemotherapy. The traditional celebration with peers was replaced by a small gathering with her oncologist, Dr. Megan, and the nursing staff. This moment marked the beginning of an eight-month intensive treatment journey that would test the limits of modern medicine and the family’s emotional endurance.
Innovative Treatment Strategies: The Role of Compassionate Use
Standard treatment protocols for pediatric AML typically involve multiple, month-long hospitalizations for high-dose chemotherapy, which often leaves the patient’s immune system severely compromised and requires constant monitoring in a sterile environment. Recognizing the aggressive nature of Emma’s specific phenotype and the potential toll of standard care, her medical team and parents opted for a different approach facilitated by "compassionate use" protocols.

Compassionate use, also known as expanded access, is a regulatory pathway that allows patients with immediately life-threatening conditions to gain access to investigational medical products outside of clinical trials when no comparable alternative therapy options are available. In Emma’s case, this allowed her to receive newer, targeted drugs that were less debilitating than standard chemotherapy.
The impact of this decision was significant for Emma’s quality of life. Unlike many children undergoing AML treatment who spend the majority of their time in hospital corridors, Emma was able to spend much of her summer at home. She continued to play soccer and spend time on the playground with her sister, Nora. According to her medical team, maintaining this level of physical activity and normalcy contributed to her overall strength, leading one doctor to remark that they had rarely seen a child fare so well under such a rigorous diagnosis.
Chronology of Treatment and the Bone Marrow Transplant Milestone
Emma’s treatment timeline was a calculated progression designed to achieve remission and prepare her body for a definitive intervention. Following five months of chemotherapy, which she managed with remarkable resilience, Emma moved toward the most critical phase of her journey: a bone marrow transplant (BMT).
A bone marrow transplant is an intensive procedure where a patient’s diseased bone marrow is replaced with healthy stem cells. The process involves "conditioning," a period of high-dose chemotherapy or radiation to eliminate the remaining cancer cells and suppress the immune system so it will not reject the donor cells. In October 2025, Emma reached the "Day +100" milestone post-transplant. In the world of transplant medicine, the 100-day mark is considered a pivotal threshold; it is the period during which the risk of acute graft-versus-host disease (GVHD) and major infectious complications is at its highest. Successfully surpassing this mark indicated that the new cells had likely engrafted and begun producing healthy blood.
Over the course of eight months, Emma spent a total of 67 nights in the hospital—a figure significantly lower than the average for her diagnosis, thanks to the outpatient-compatible nature of her experimental treatment. Despite this success, the journey remains ongoing. Emma is currently in a maintenance phase, requiring a regimen of multiple medications and frequent follow-up appointments that will continue for at least the next two years to monitor for recurrence.
The "Celebrate Everything" Philosophy and the Psychological Impact of Milestones
In pediatric oncology, the tradition of "ringing the bell" usually signifies the end of all active treatment. However, Ashley and Jacob adopted a different approach, choosing to "ring multiple bells" for every small victory. This philosophy—celebrate everything—was born out of the reality that a final "finish line" is never guaranteed with a 15% survival rate.
By celebrating every step—from a successful round of meds to a good blood count report—the family shifted the focus from the looming threat of the disease to the tangible successes of the present. This approach is supported by psychological research into "resilience-based care," which suggests that acknowledging small milestones can reduce the trauma associated with long-term medical treatment for both the child and the caregivers.
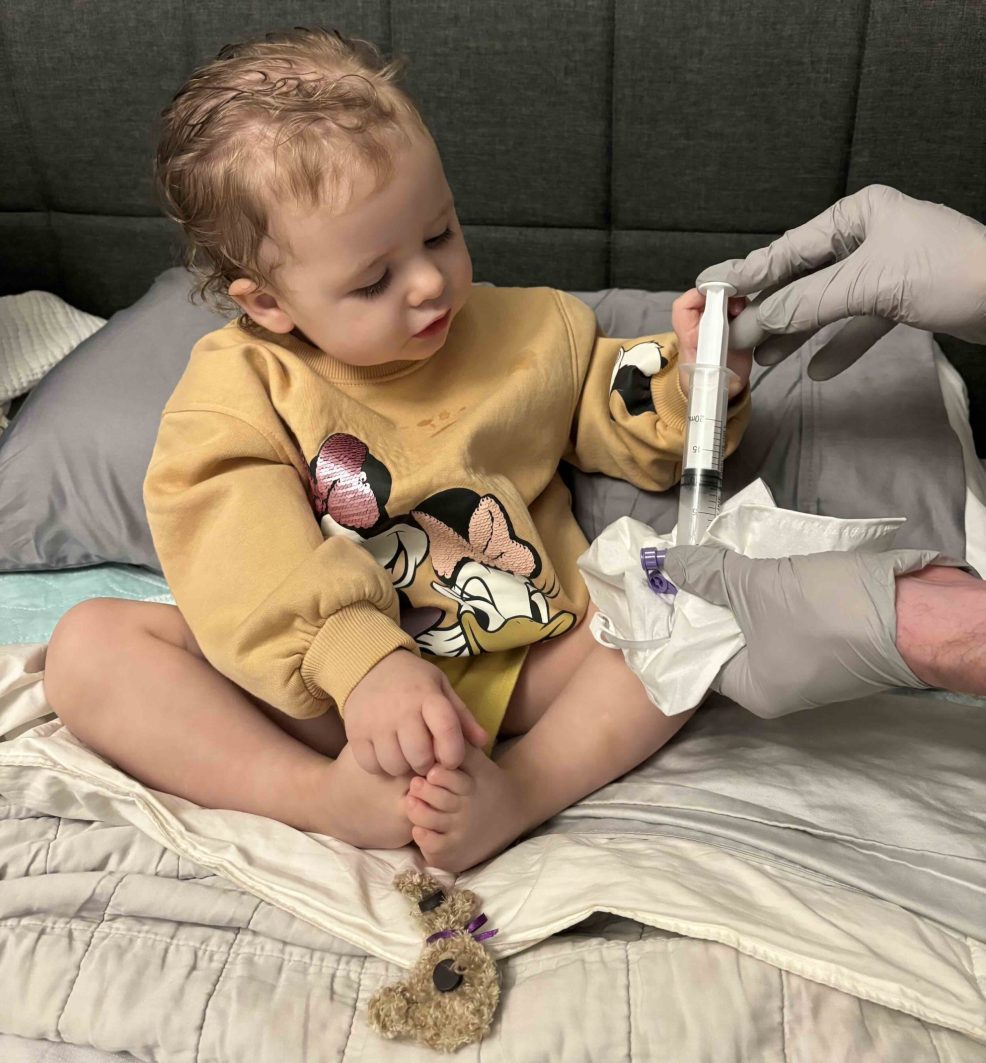
For Emma, these celebrations were woven into a childhood that has become inextricably linked with her medical care. Her comfort objects include "hospital socks" and a stuffed animal named Asha, named after a therapy dog at the hospital. Her ability to greet doctors as family and maintain a cheerful disposition, often telling staff, "See you later, alligator," reflects a successful integration of her medical reality into her social development.
Community Support and the Social Safety Net
The burden of childhood cancer extends beyond the patient to the entire family unit, often resulting in financial strain and emotional exhaustion. In Emma’s case, a network of community support provided essential relief. The local nonprofit "Wishes and More" installed a swing set in the family’s backyard, providing a safe space for Emma to play during her recovery.
Furthermore, community members organized a "craft train," ensuring that Emma and Nora had a steady supply of activities to keep them engaged during periods of isolation. Even small gestures, such as a loaf of sourdough bread from Emma’s uncle, played a role in her recovery; it was the first solid food she felt motivated to eat during a particularly difficult week of treatment. These interventions highlight the importance of holistic support systems in pediatric oncology, where the goal is not just survival, but the preservation of childhood.
Broader Implications: The Pediatric AML Collaborative and Research Funding
Emma’s improved prognosis—now estimated by her doctors to be near 50%, a significant jump from the baseline 15%—is a direct result of clinical research and the availability of experimental therapies. However, her story also highlights the ongoing need for more targeted research into rare pediatric leukemias.
To address this need, the Children’s Cancer Research Fund (CCRF) recently launched the Pediatric AML Collaborative. This national coalition brings together families, clinicians, and researchers to create a unified scientific strategy. The goal is to move away from fragmented research efforts and toward a coordinated model that can accelerate the development of treatments specifically for high-risk phenotypes like AML-RAM.

The implications of such research are profound. Currently, pediatric cancer research receives only about 4% of federal funding for cancer research in the United States. Foundations and private collaboratives are increasingly filling this gap, focusing on precision medicine and genomic sequencing to identify why certain leukemias are resistant to standard care. Emma’s case serves as a "proof of concept" for this movement: when research is funded and experimental drugs are made accessible, survival rates can more than triple.
Analysis of the Road Ahead
While Emma’s progress is extraordinary, the medical reality remains sober. She continues to take more medications than can be counted on one hand, each carrying risks of long-term side effects, including potential impacts on heart health, fertility, and secondary cancers. The "road" that Ashley speaks of laying down in front of her daughter is one paved with continuous monitoring and the hope that the next two years of maintenance therapy will keep the leukemia at bay.
The shift in Emma’s survival odds from 15% to 50% represents a monumental victory in the field of pediatric oncology, yet it also underscores the work left to be done. A 50% survival rate still means that half of the children with this diagnosis do not survive. The momentum generated by cases like Emma’s is critical for maintaining public interest and funding for the Pediatric AML Collaborative.
As the family plans trips to apple orchards and navigates a whiteboard filled with medical appointments, their story serves as a dual message to the public and the medical community. It is a message of hope that "impossible" odds are being rewritten by science, and a call to action that for many children still waiting for their "first bell," the research cannot move fast enough. Through the lens of Emma’s "celebrate everything" motto, every day of health is a hard-won victory and a testament to the power of medical innovation.

