In the specialized field of pediatric oncology, the diagnosis of a diffuse midline glioma (DMG) has historically been regarded as one of the most challenging and devastating clinical outcomes. However, a landmark clinical trial that opened in early 2025 at Children’s Minnesota is seeking to alter the trajectory of this disease. Rooted in more than two decades of rigorous laboratory research and academic collaboration, the trial represents a significant shift in how the medical community approaches incurable pediatric brain tumors. Led by oncologist and researcher Chris Moertel, MD, and his colleague Michael Olin, PhD, from the University of Minnesota, the study investigates a novel immunotherapy combination designed to dismantle the biological defenses of aggressive tumors, potentially offering patients what their families value most: more time.
The Biological Challenge of Diffuse Midline Glioma
Diffuse midline glioma, which includes the condition formerly known as Diffuse Intrinsic Pontine Glioma (DIPG), is a high-grade primary brain tumor that occurs in the critical midline structures of the brain, such as the pons, thalamus, and spinal cord. Because these tumors infiltrate healthy brain tissue and are located in areas responsible for vital functions like breathing, heart rate, and motor control, surgical resection is almost never a viable option.
Current standard-of-care treatments typically involve focal radiation therapy, which can temporarily shrink the tumor and alleviate symptoms but is rarely curative. Historically, most children diagnosed with DMG face a median survival rate of nine to 13 months post-diagnosis. The primary obstacle to effective treatment has been the tumor’s ability to evade the human immune system. Research by Drs. Olin and Moertel identified that these tumors produce a specific protein that functions as a sophisticated "shield," preventing T-cells and other immune responders from recognizing or attacking the malignant cells.

A Two-Decade Chronology of Research and Discovery
The clinical trial launched in 2025 is the culmination of twenty years of persistent investigation at the University of Minnesota. The journey began in the early 2000s, focusing on the molecular mechanisms of immune evasion in glioblastomas and other high-grade gliomas.
- Initial Discovery (2005–2012): Dr. Michael Olin and his team identified the specific peptide and protein interactions that allowed brain tumors to remain "invisible" to the immune system. They discovered that the tumor secretes a suppressive factor that effectively deactivates local immune responses.
- Peptide Development (2013–2018): Researchers focused on engineering a synthetic peptide capable of neutralizing this protective shield. This "shield-busting" molecule was designed to be administered alongside other therapies to heighten the body’s natural defenses.
- Preclinical Success (2019–2023): Extensive laboratory testing and animal models demonstrated that when the protective barrier was compromised, the immune system could successfully target and reduce tumor mass. These results paved the way for human clinical trials.
- Trial Launch (Early 2025): The Phase I/II clinical trial opened at Children’s Minnesota. This trial, co-led by Dr. Anne Bendel and Dr. Maggie Skrypek, utilizes a new vaccine in combination with the shield-busting molecule developed by Olin and Moertel.
The funding for this extensive research trajectory was provided in large part by the Children’s Cancer Research Fund (CCRF), a non-profit organization that specializes in bridging the gap between initial laboratory discoveries and clinical implementation.
The Case of Eva: From Diagnosis to Enrollment
The human impact of this scientific progress is best illustrated by the experiences of families who have exhausted traditional medical options. In January 2025, an eight-year-old girl named Eva began exhibiting subtle neurological symptoms. During a typical afternoon, her parents, Lee and Sandra, noticed a slight drooping on one side of her face.
Initial medical consultations at an emergency room suggested Bell’s palsy, a relatively common condition involving temporary facial muscle weakness. However, during a subsequent routine physical, a pediatrician noted that Eva had lost hearing in one ear. A follow-up MRI revealed a large mass in the midline of her brain. The diagnosis was confirmed as DMG, and the prognosis was the standard, heartbreaking timeline of less than a year.
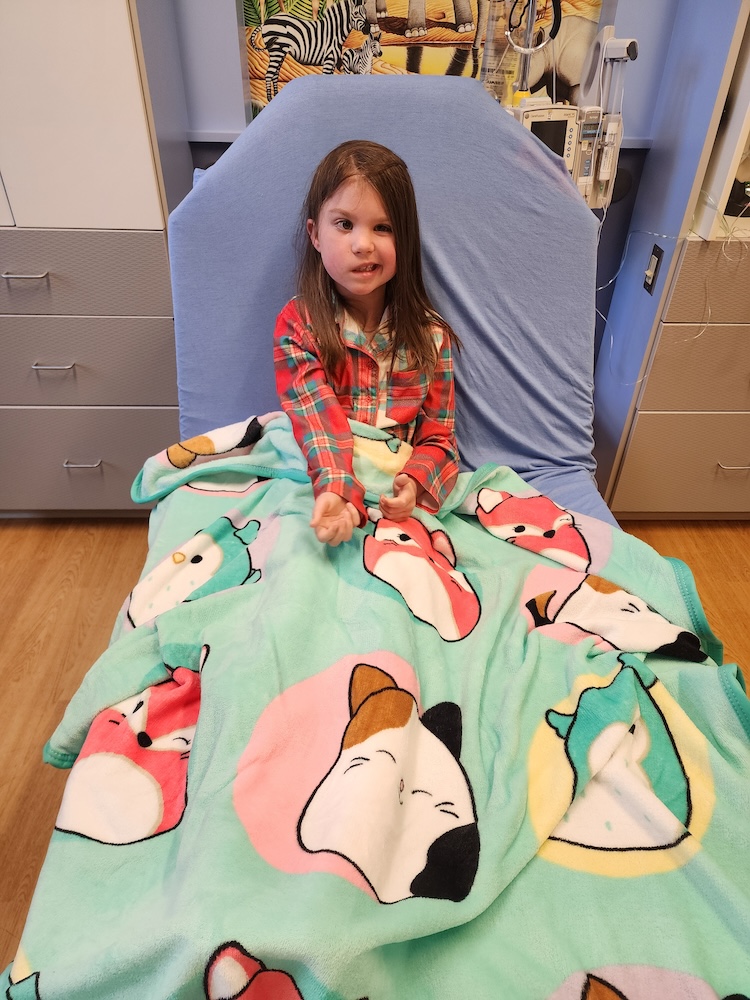
By May 2025, Eva’s family made the decision to enroll her in the CCRF-funded clinical trial at Children’s Minnesota. For families like Eva’s, the trial represents a shift from purely palliative care to active participation in a potential medical breakthrough.
Clinical Framework and Methodology of the Trial
The trial is designed to test the safety and efficacy of a dual-action immunotherapy protocol. Unlike traditional chemotherapy, which utilizes cytotoxic chemicals to kill rapidly dividing cells (often causing significant collateral damage to healthy tissue), this immunotherapy approach is more targeted.
The treatment involves multiple injections per month, typically ranging from two to four doses per session. The protocol consists of:
- The Shield-Busting Molecule: A synthetic peptide that targets the immunosuppressive proteins produced by the tumor. By neutralizing these proteins, the molecule "unmasks" the tumor to the patient’s immune system.
- The Therapeutic Vaccine: A vaccine designed to prime the immune system to recognize specific antigens associated with DMG cells.
A critical aspect of this trial is the preservation of the patient’s quality of life. Traditional high-dose radiation and chemotherapy often result in severe fatigue, nausea, and cognitive decline. In contrast, the immunotherapy injections administered in this study have shown a lower toxicity profile. For Eva, this has meant the ability to remain active in her daily life, continuing to attend school and participate in her passion for dance, despite the severity of her underlying condition.

Statistical Context and the Role of Philanthropy
Pediatric brain tumors are the leading cause of cancer-related death in children. While survival rates for certain pediatric cancers, such as acute lymphoblastic leukemia, have risen to nearly 90%, the survival rate for DMG has remained largely unchanged for over four decades.
One of the primary reasons for this stagnation is the "funding gap." Because pediatric brain tumors are considered rare—affecting roughly 300 to 400 children in the United States annually—large pharmaceutical companies often find little financial incentive to invest in the necessary research and development. This is where organizations like the CCRF play a vital role. By providing consistent, long-term funding for researchers like Drs. Moertel and Olin, philanthropic groups allow for the high-risk, high-reward research that federal grants may overlook.
The CCRF’s involvement in the University of Minnesota’s brain tumor program has been a cornerstone of this 20-year journey. Without private donor support, the transition from the laboratory bench to the patient’s bedside at Children’s Minnesota would likely have faced significant delays or remained unfunded entirely.
Broader Implications for Pediatric Oncology
The implications of this trial extend beyond the specific treatment of DMG. If the "shield-busting" peptide proves successful in human subjects, the technology could theoretically be adapted for other types of solid tumors that utilize similar immune-evasion tactics. This includes other high-grade pediatric gliomas and potentially certain adult cancers.

Dr. Anne Bendel, one of the trial’s co-leaders, emphasizes that every patient enrolled provides invaluable data. Even in cases where the treatment may not result in a total cure, the biological feedback regarding how the immune system reacts to the vaccine allows researchers to "tweak" and refine the protocol for future cohorts. This iterative process is the standard pathway toward turning an "incurable" disease into a manageable or curable one.
Conclusion: A Legacy of Time and Science
As the trial progresses through 2025, the medical community remains cautiously optimistic. For the families currently enrolled, the goal is "the gift of time"—more birthdays, more school days, and more memories. For the researchers, the goal is the eventual eradication of DMG as a terminal diagnosis.
Dr. Moertel’s career has been defined by the pursuit of these extra months and years for his patients. "If we can break down the tumor’s barrier to allow the immune system to do its job, then we are well on the way to helping cure those kids," he stated during the trial’s opening.
The story of Eva and the decades of research by Olin and Moertel underscore a pivotal moment in pediatric medicine. While the road to a universal cure for brain cancer remains long, the 2025 clinical trial at Children’s Minnesota marks a definitive step forward, fueled by scientific persistence and the hope of families who refuse to accept the status quo. Through the participation of current patients, a legacy is being built that may ensure that in the future, no parent has to hear that their child’s time is running out.

