The American Cancer Society’s (ACS) highly anticipated Cancer Statistics 2026 report paints a compelling picture of both remarkable progress and enduring challenges in the fight against cancer. This authoritative annual publication, drawing on comprehensive data from sources like the National Cancer Institute’s Surveillance, Epidemiology, and End Results (SEER) program and the Centers for Disease Control and Prevention’s National Program of Cancer Registries (NPCR), serves as a vital benchmark for understanding the nation’s cancer landscape. Its latest findings highlight a historic surge in survival rates, largely attributed to revolutionary scientific breakthroughs, particularly in the fields of immunotherapy and targeted treatments, which are now extending lives once deemed beyond saving.
A Historic Leap in Survival
The headline finding of the 2026 report is the unprecedented achievement in overall cancer survival. In the United States, the five-year relative survival rate for all cancers combined has reached a historic milestone of 70% during the period of 2015–2021. This represents a monumental leap from just 49% in the mid-1970s, underscoring nearly five decades of sustained effort in research, prevention, and treatment. This dramatic improvement translates into millions of lives extended and countless families spared the immediate grief of cancer loss. Perhaps most striking are the profound gains observed in the survival rates for advanced, metastatic cancers—those that have spread beyond their primary site—which were frequently considered untreatable just a generation ago. These improvements signify not marginal shifts, but fundamental changes in the prognosis for patients facing the most aggressive forms of the disease.
The steady decline in cancer mortality is further evidenced by the report’s revelation that from 1991 to 2023, the cancer death rate in the U.S. decreased by an impressive 34%. This translates to an estimated 4.8 million cancer deaths averted over this period, a testament to multifaceted progress. Key drivers behind this reduction include a significant decrease in smoking rates, which has profoundly impacted lung cancer incidence and mortality; advancements in early detection methods, such as improved screening for breast, colorectal, and cervical cancers; and, crucially, the continuous evolution and refinement of cancer treatments, with immunotherapy emerging as a game-changer.
The Enduring Burden: Cancer by the Numbers
Despite these encouraging trends, cancer remains a formidable public health challenge. The report reiterates that cancer is the second leading cause of death in the U.S. overall. For specific demographics, however, its impact is even more pronounced: it stands as the leading cause of death for men aged 60–79 and women aged 40–79.

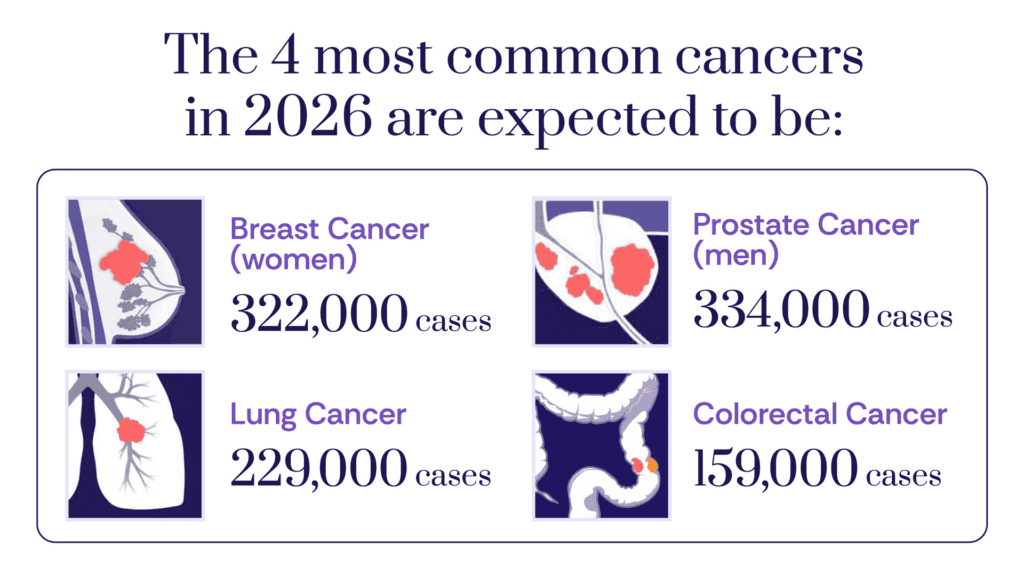
For the year 2026, the ACS estimates that approximately 2.1 million Americans will receive a cancer diagnosis, with an estimated 626,000 deaths. These figures translate to a staggering daily toll of about 5,800 new cancer cases and 1,720 deaths, underscoring the relentless prevalence and lethality of the disease. Among the various cancer types, lung cancer continues to be the deadliest, projected to cause more deaths than the second- and third-deadliest cancers—colorectal and pancreatic—combined. This grim statistic highlights the urgent need for continued efforts in lung cancer prevention, early detection, and the development of more effective therapies, particularly given its strong link to tobacco use, though non-smokers can also develop the disease.
Immunotherapy: Rewriting Survival Curves
The Cancer Statistics 2026 report prominently features the transformative impact of immunotherapy and targeted therapies. These breakthrough treatments are documented as the primary drivers behind the extraordinary five-year survival gains across several advanced cancers. Unlike traditional treatments such as chemotherapy, which broadly attack rapidly dividing cells, or radiation, which targets localized tumors, immunotherapies harness the body’s own immune system to recognize and destroy cancer cells. Targeted therapies, on the other hand, focus on specific molecular pathways that are crucial for cancer growth and survival, often with fewer side effects than conventional chemotherapy.
The evolution of immunotherapy marks a paradigm shift in oncology. Decades of fundamental research into how the immune system functions and how cancer evades it laid the groundwork for these therapies. A pivotal moment came with the development of immune checkpoint inhibitors, such as anti-PD-1 and anti-CTLA-4 therapies. These drugs work by blocking specific proteins (checkpoints) that cancer cells use to switch off immune responses, thereby "releasing the brakes" on the immune system and allowing it to attack the tumor.
Antoni Ribas, MD, PhD, a distinguished Professor at UCLA and a member of the Cancer Research Institute (CRI) Scientific Advisory Council, emphasizes this profound impact: “When we look at metastatic melanoma survival improving from 16% to 35% in just 25 years, we’re witnessing the direct impact of immune checkpoint inhibitors like anti-PD-1 and anti-CTLA-4 therapies. These are the breakthroughs that the Cancer Research Institute has championed for decades – supporting the fundamental science that made immunotherapies a reality.” This dramatic improvement in metastatic melanoma, once considered a death sentence, is mirrored in other aggressive cancers. For instance, advanced kidney cancer and certain types of lung cancer have also seen significant improvements in survival rates with the advent of immunotherapy, transforming patient outlooks from months to years. The sustained investment in basic immunology research by organizations like CRI and the National Cancer Institute (NCI) has been instrumental in translating complex scientific discoveries into life-saving treatments.
Progress, While Real, Remains Uneven
Despite the celebratory tone surrounding overall survival gains, the report also serves as a stark reminder that progress in the cancer fight has been, and continues to be, uneven. Significant disparities persist across various demographic groups and geographic regions, underscoring the urgent need for sustained research, innovative policy interventions, and equitable healthcare delivery.
Rising Cancer Rates Among Young Adults: The report highlights a concerning trend of rising cancer rates in younger adults. While specific data points were not detailed in the original summary, broader epidemiological studies have shown an increase in certain cancers, such as colorectal cancer, pancreatic cancer, and some gynecological cancers, among individuals under the age of 50. This trend challenges previous assumptions about cancer predominantly being a disease of older age and points to potential shifts in environmental factors, lifestyle choices, or even changes in diagnostic practices. The implications are profound, affecting individuals at critical life stages, impacting fertility, career development, and long-term health. Addressing this requires a deeper understanding of unique risk factors in younger populations and tailored prevention and early detection strategies.
Widening Geographic Gaps: Access to high-quality cancer care is not uniformly distributed across the United States. The report notes widening geographic gaps, which often correlate with socioeconomic status and rurality. Patients in rural areas frequently face significant barriers, including longer travel distances to specialized cancer centers, shortages of oncology specialists, limited access to advanced diagnostic technologies, and fewer opportunities to participate in clinical trials. These disparities can lead to later diagnoses, less comprehensive treatment plans, and ultimately, poorer outcomes compared to their urban counterparts. Bridging these gaps necessitates investments in telehealth infrastructure, mobile screening units, and programs designed to incentivize oncologists to practice in underserved regions.
Persistent Racial and Ethnic Inequities: Perhaps the most sobering aspect of the report is its emphasis on persistent racial and ethnic inequities in cancer outcomes. These disparities are not merely statistical anomalies but are deeply rooted in systemic barriers that permeate the healthcare system and broader society. The report explicitly states that these inequities stem from a “higher prevalence of risk factors, medical mistrust, and lack of insurance, which hinders access to high-quality health care.”
Even after meticulously controlling for factors like stage at diagnosis and socioeconomic status, survival gaps stubbornly remain. The “largest contributor” to these enduring disparities is identified as “less access to high-quality care across the cancer continuum, from prevention to diagnosis and treatment.” For instance, African American men face higher incidence and mortality rates for prostate cancer compared to white men, and Black women often experience higher mortality from breast cancer despite similar incidence rates. These disparities are exacerbated by historical and ongoing systemic racism, leading to medical mistrust, implicit bias in care delivery, and unequal distribution of resources. Social determinants of health, such as stable housing, nutritious food, safe environments, and educational opportunities, also play a critical role, disproportionately affecting marginalized communities and contributing to a higher burden of risk factors. Addressing these inequities demands comprehensive, community-centered approaches that build trust, expand insurance coverage, diversify the healthcare workforce, and dismantle systemic barriers to care. Organizations like the NCI have increasingly focused on health equity initiatives, recognizing that medical advancements must reach all populations to achieve true progress.
The Road Ahead: Sustaining Momentum and Tackling Intractable Cancers
The Cancer Statistics 2026 report stands as a powerful testament to the efficacy of sustained scientific research. The immunotherapy revolution, with its profound impact on patient survival, did not materialize overnight. It was meticulously built upon decades of foundational basic science, generously funded by institutions like the National Cancer Institute and critical philanthropic organizations such as the Cancer Research Institute. These long-term investments in understanding fundamental biological processes have been the bedrock upon which translational breakthroughs have been built.
However, the very data that celebrates monumental progress also starkly illuminates how far the journey must still extend. Certain cancers continue to defy significant improvements in survival, representing critical areas for intensified research. Pancreatic cancer, for example, remains one of the most lethal malignancies, with its five-year survival rate stagnant at a dismal 13%. This means that for an estimated 185 Americans diagnosed with pancreatic cancer each day, their odds of survival have essentially remained unchanged for decades. The challenge with pancreatic cancer lies in its aggressive nature, late-stage diagnosis due to often vague symptoms, and inherent resistance to many conventional therapies. Future research must focus on earlier detection biomarkers, novel drug targets, and more effective combination therapies to make a dent in these stubbornly low survival rates.

Concurrently, the report notes a disturbing trend: uterine corpus cancer mortality continues its alarming 26-year climb. This rise is particularly concerning and may be linked to increasing rates of obesity, which is a known risk factor for this type of cancer, as well as potential changes in diagnostic patterns or access to optimal care. Understanding the multifactorial reasons behind this upward trajectory is paramount for developing effective prevention and treatment strategies.
The implications for the field of immunotherapy are clear: while incredibly successful in many contexts, the work is far from over. The documented survival gains validate past investments, but they also underscore the imperative to expand the reach and effectiveness of immunotherapies. This means investigating why some patients respond dramatically while others do not, overcoming mechanisms of resistance, and developing next-generation immunotherapies. Research into combination therapies (immunotherapy with chemotherapy, radiation, or targeted drugs), the development of advanced cellular therapies like CAR T-cells for solid tumors, and the exploration of cancer vaccines are all critical avenues for future progress.
The ultimate vision articulated by the report and championed by the broader cancer research community is clear: every patient, regardless of their diagnosis, deserves access to the latest, most effective advances in immunotherapy and cancer care. Furthermore, every cancer type, including those with currently grim prognoses, deserves the sustained and robust research investment necessary for breakthrough discoveries. Crucially, the fight against cancer must also be a fight for equity: every community, irrespective of race, ethnicity, or socioeconomic status, deserves equal access to life-saving cancer prevention, diagnosis, and treatment.
The human immune system possesses an extraordinary, yet still largely untapped, power to combat cancer. Continued, innovative research, supported by robust funding and a commitment to health equity, is not merely beneficial; it is absolutely essential to fully unlock this power and extend its transformative promise to patients in every corner of the nation and beyond.

