Luke Schoenbauer, a doctoral candidate in the physical therapy program at the University of Minnesota, possesses a unique clinical perspective that few of his peers can claim. When he walks across the clinical floor, his gait is powered by a prosthetic limb—a visible reminder of a decade-long battle with pediatric bone cancer. For Schoenbauer, the prosthesis is not merely a medical device but a conversational bridge and a teaching tool. As he nears his graduation in May, his journey from a nine-year-old oncology patient to a healthcare provider offers a profound look into the complexities of osteosarcoma treatment, the surgical innovation of rotationplasty, and the critical importance of psychological normalcy in pediatric recovery.
The Pathological Fracture: A Red Flag in Pediatric Medicine
The trajectory of Schoenbauer’s life shifted fundamentally during a routine moment of childhood play. At age eight, while roughhousing with his older brothers, a relatively minor fall from a couch resulted in an audible "crack" that signaled a catastrophic injury. Schoenbauer recalls the immediate realization that his leg was no longer structurally sound, observing a wave of nausea as he witnessed part of his limb move independently of the rest.
Upon arrival at the emergency department, medical imaging confirmed a fracture of the femur. In the field of orthopedics, the femur is recognized as the longest, heaviest, and strongest bone in the human body. A fracture resulting from low-energy trauma—such as a fall from a couch—is classified as a "pathological fracture." This term indicates that the bone was already weakened by an underlying disease process, making it susceptible to breaks that would not occur in healthy tissue.
While surgeons initially stabilized the leg using external fixation—a series of metal pins connected to an external frame—the diagnostic focus shifted toward why the bone had failed. Subsequent scans revealed a cyst-like lesion within the femur. Three months later, when the bone failed to show expected signs of healing, a biopsy was performed. The results were definitive: Schoenbauer was diagnosed with osteosarcoma.

Understanding Osteosarcoma: Statistics and Clinical Challenges
Osteosarcoma is the most common type of bone cancer in children and adolescents, though it remains a rare disease in the broader population. According to data from the American Cancer Society, approximately 800 to 1,000 new cases are diagnosed annually in the United States, with about half of these occurring in children and teens. The disease typically originates in the "growth plates" near the ends of long bones, most frequently around the knee (the distal femur or proximal tibia) or the shoulder (proximal humerus).
The discovery of Schoenbauer’s cancer via a fracture is a common, albeit traumatic, diagnostic path. For many patients, the tumor remains asymptomatic or causes dull aches often dismissed as "growing pains" until the bone’s structural integrity is compromised. At the time of his diagnosis, Schoenbauer’s clinical team faced a dual challenge: eradicating a highly aggressive malignancy while attempting to preserve as much mobility as possible for an active young boy.
The Pivotal Choice: Rotationplasty Versus Limb Salvage
Following initial rounds of intensive chemotherapy designed to shrink the tumor, Schoenbauer and his family were presented with a difficult surgical choice. The standard options for high-grade osteosarcoma of the femur typically include limb-salvage surgery or amputation.
Limb-salvage surgery involves removing the cancerous bone and replacing it with a metal prosthesis or a bone graft. While this preserves the appearance of the limb, it often comes with significant long-term restrictions on physical activity and a higher risk of local recurrence or mechanical failure of the implant. The second option, a traditional above-knee amputation, would offer a higher clearance of the cancer but would significantly limit the patient’s mobility, as controlling a prosthetic knee joint is biologically demanding and less efficient.
The surgical team suggested a third, more specialized option: rotationplasty, also known as a Van Nes rotation. In this complex procedure, the portion of the leg containing the tumor (the knee and distal femur) is removed. The lower leg and foot are then rotated 180 degrees and reattached to the remaining upper femur. This configuration allows the ankle joint to function as a knee joint. When fitted with a prosthesis, the heel becomes the "kneecap," and the foot fits into the prosthetic socket, allowing the patient to use their own calf muscles and ankle flexors to control the limb.
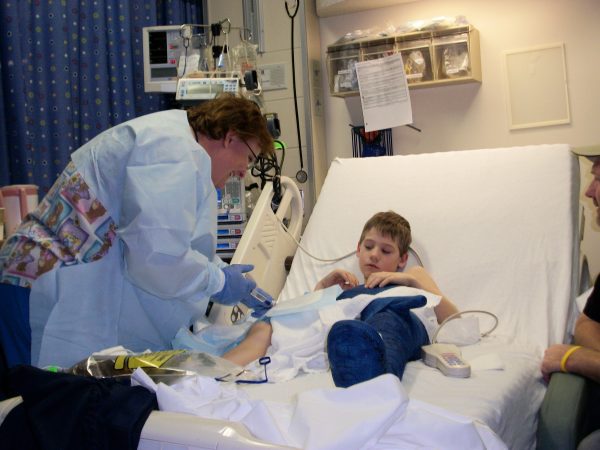
For an athletic child like Schoenbauer, rotationplasty offered the best chance for a return to high-impact activities. Despite the unconventional aesthetic of a backward-facing foot, the functional benefits—such as the ability to run, jump, and play sports with greater ease than a traditional amputee—led the family to choose this path.
The Long Road of Recovery and Recurrence
The recovery process was far from linear. Schoenbauer spent significant portions of his third and fourth-grade years utilizing wheelchairs and walkers. The physical toll of the surgery was compounded by continued chemotherapy, which left him in a state of chronic fatigue and physical weakness.
"Getting used to the prosthesis was hard," Schoenbauer noted, reflecting on the discomfort of the early fittings and the steep learning curve of retraining his brain to use his ankle as a knee.
Just as he began to regain his independence, the cancer followed a common and deadly pattern. Osteosarcoma has a high propensity for metastasis, most frequently spreading to the lungs. Schoenbauer faced two separate pulmonary recurrences over the following years. Each instance required surgical intervention to remove the tumors, and the second recurrence necessitated another three-month course of chemotherapy.
The ten-year milestone of being cancer-free, which Schoenbauer recently celebrated, is a significant clinical benchmark. In pediatric oncology, the risk of recurrence drops substantially after five years of remission, though the psychological "scanxiety"—the fear associated with follow-up imaging—often persists for a lifetime.
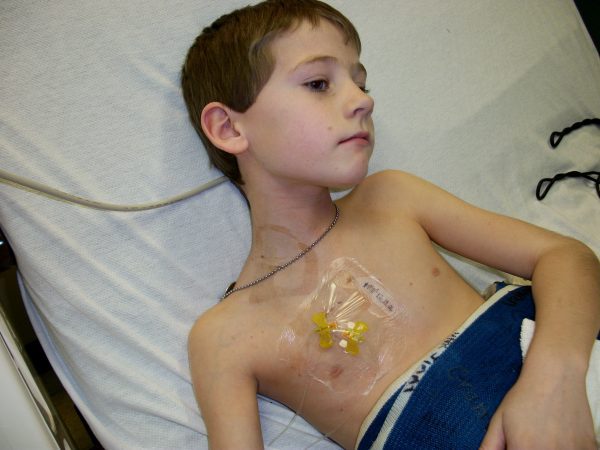
From Patient to Provider: The University of Minnesota and Beyond
Schoenbauer’s transition from the oncology ward to the University of Minnesota’s physical therapy program represents a full-circle moment in his medical journey. His background as a patient provides him with an empathetic "shorthand" when dealing with individuals facing limb loss or chronic illness.
This unique perspective has been particularly impactful in his volunteer work with the Protez Foundation. This Minnesota-based non-profit organization provides prosthetic care, rehabilitation, and psychological support for Ukrainians who have lost limbs due to the ongoing conflict in their home country.
In the clinical setting with Ukrainian soldiers and civilians, Schoenbauer’s prosthetic leg serves as a powerful symbol of possibility. "Sometimes I’ll see a patient notice my prosthetic, and that creates a connection," he explained. For someone who has recently undergone a traumatic amputation, seeing a healthcare provider who walks with a fluid gait and understands the mechanical nuances of a socket fit can be more encouraging than any clinical lecture.
The Psychological Importance of Normalcy in Pediatric Care
Beyond the surgical and rehabilitative aspects of his story, Schoenbauer emphasizes a critical, often overlooked component of pediatric oncology: the social environment. He advocates for treating children with cancer with as much "normalcy" as possible.
During his treatment, Schoenbauer found the greatest relief not in the specialized care of adults, who were often overly gentle or somber, but in the company of friends who treated him as they always had. He recalls the value of playing video games with peers—an activity where his physical limitations were irrelevant, and he could compete on equal footing.

"As a kid with cancer, every single person around you starts to treat you differently," Schoenbauer said. "I’d say if you can find a way to give [normalcy] to a kid going through this, that’s the best way to help."
Broader Implications for Pediatric Oncology and Rehabilitation
Luke Schoenbauer’s case highlights several evolving trends in the treatment of pediatric bone cancers. First, it underscores the success of multidisciplinary care—combining aggressive surgery, personalized chemotherapy, and long-term physical therapy. Second, it demonstrates the long-term viability of rotationplasty as a functional alternative to traditional amputation, particularly for patients who wish to remain physically active.
Furthermore, his story reflects a growing movement in healthcare toward "expert patients"—individuals who use their lived experience with chronic or catastrophic illness to inform their professional practice. As Schoenbauer prepares to graduate and enter the workforce as a licensed physical therapist, he joins a specialized group of providers who can bridge the gap between clinical theory and the lived reality of disability.
The implications of his journey extend to the global stage through his work with the Protez Foundation, highlighting how local medical expertise in Minnesota can impact international humanitarian efforts. As the field of prosthetics continues to advance with microprocessor joints and osseointegration, the human element—the relationship between the therapist and the patient—remains the cornerstone of successful rehabilitation. Schoenbauer’s career is poised to be a testament to that enduring truth, proving that while cancer may have changed the structure of his leg, it served to strengthen the foundation of his future as a healer.

