Luke Schoenbauer, a doctoral candidate in the physical therapy program at the University of Minnesota, possesses a clinical perspective that few of his peers can claim. When Schoenbauer walks through the halls of the university or treats patients in clinical rotations, he is acutely aware of the subtle glances directed toward his lower leg. As an amputee since the age of nine, he has developed a keen intuition for the curiosity of others, often sensing the questions they are hesitant to voice. Rather than recoiling from this scrutiny, Schoenbauer embraces it as a cornerstone of his professional and personal identity. His journey from a pediatric oncology patient to a future healthcare provider offers a profound look at the intersection of medical innovation, personal resilience, and the evolving landscape of pediatric cancer survivorship.
The trajectory of Schoenbauer’s life changed fundamentally during what should have been a routine moment of childhood play. At eight years old, while wrestling with his older brothers, a relatively minor fall from a couch resulted in an audible crack that signaled a catastrophic injury. The subsequent realization that he had fractured his femur—the longest, strongest bone in the human body—immediately raised clinical red flags. A femur fracture in a healthy child typically requires high-impact trauma, such as a motor vehicle accident or a significant fall from height. When such a bone breaks during low-impact activity, it is often classified as a pathological fracture, suggesting the bone was already compromised by an underlying condition.
Emergency room physicians at the time utilized metal pins and an external fixator to stabilize the limb, but diagnostic imaging revealed a more sinister cause for the bone’s fragility: a cyst-like growth within the femur. Three months of poor healing prompted a biopsy, which confirmed a diagnosis of osteosarcoma. Osteosarcoma is a primary bone malignancy that most frequently occurs in children and young adults, typically during periods of rapid growth. According to data from the National Cancer Institute, osteosarcoma accounts for approximately 3% of all childhood cancers, with about 800 to 900 new cases diagnosed annually in the United States.

The Clinical Challenge of Osteosarcoma
The diagnosis of osteosarcoma presents a complex set of surgical and oncological challenges. In Schoenbauer’s case, the cancer had so thoroughly weakened the femoral structure that the fracture was inevitable. His treatment required a multi-modal approach involving aggressive chemotherapy and a definitive surgical intervention to remove the primary tumor. For pediatric patients, the choice of surgery is a life-altering decision. Schoenbauer was presented with two primary options: a limb-salvage procedure involving the insertion of a metal rod to replace the affected bone, or an amputation.
Limb-salvage surgery, while aesthetically preserving the appearance of the leg, often carries a higher risk of local recurrence and may require multiple follow-up surgeries as the child grows. Conversely, amputation offers a higher statistical probability of complete tumor clearance. Schoenbauer’s medical team, in consultation with his parents, ultimately deferred the final decision to the nine-year-old himself. He opted for a specialized and rare procedure known as rotationplasty.
In a rotationplasty, the middle portion of the leg (including the knee) is removed. The lower leg and foot are then rotated 180 degrees and reattached to the upper thigh. This allows the ankle joint to function as a knee joint, pointing forward. This surgical configuration provides the patient with a functional "knee" that can be fitted with a prosthetic, allowing for a level of athletic activity and mobility that traditional above-knee amputations rarely afford. While the procedure results in a unique physical appearance, its functional outcomes are often superior for active children.
A Decade of Resilience and Recurrence
Schoenbauer’s recovery was far from linear. The physical demands of adapting to a prosthetic limb were compounded by the systemic exhaustion of ongoing chemotherapy. For much of his third and fourth-grade years, Schoenbauer relied on wheelchairs and walkers, navigating the social and physical hurdles of elementary school as an amputee. However, the true test of his resilience came after he had regained his ability to walk.
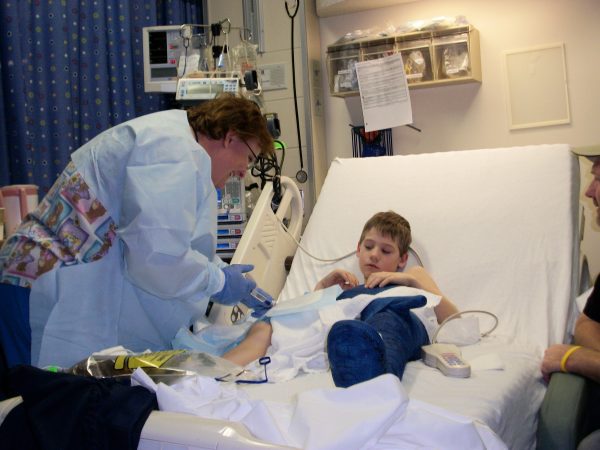
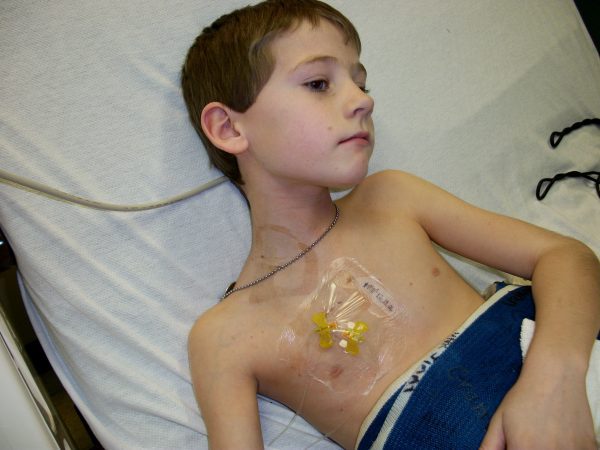
In many cases of osteosarcoma, the cancer cells migrate to the lungs, a process known as pulmonary metastasis. Despite the successful amputation, Schoenbauer faced two separate recurrences in his lungs over the following years. Each instance required surgical intervention to remove the tumors, and the second recurrence necessitated an additional three-month course of intensive chemotherapy. These setbacks are common in the clinical timeline of osteosarcoma; statistics indicate that approximately 20% to 25% of patients have detectable metastatic disease at the time of diagnosis, while others may develop it during or after treatment.
Today, Schoenbauer marks a significant milestone: ten years of being cancer-free. While he no longer requires the frequent surveillance scans that once dictated his schedule, the psychological weight of his history remains. "That thought is always there, in the back of my mind," he noted, referring to the possibility of a third recurrence. This "scanxiety"—a term often used in the survivor community—is a documented psychological phenomenon among pediatric cancer survivors, highlighting the need for long-term mental health support alongside physical rehabilitation.
Bridging the Gap Between Patient and Provider
Schoenbauer’s transition into the field of physical therapy is a natural evolution of his lived experience. Having spent years as the recipient of rehabilitative care, he is now preparing to graduate in May from the University of Minnesota’s physical therapy program. His unique perspective allows him to build immediate rapport with patients, particularly those facing limb loss.
His work with the Protez Foundation serves as a testament to this connection. The foundation provides prosthetic care and rehabilitation for Ukrainians who have lost limbs due to the ongoing conflict in their country. When Ukrainian soldiers and civilians arrive for treatment, Schoenbauer’s presence serves as a living proof of what is possible. "They can see that I know what this is like," he explained. "They’ll watch me walk, and it helps them see, ‘Okay, that’s where I can get to.’"
From a clinical standpoint, Schoenbauer’s ability to demonstrate the mechanics of prosthetic gait is invaluable. Physical therapy for amputees involves complex neuromuscular re-education, balance training, and core strengthening. By embodying the success of these interventions, Schoenbauer provides a level of motivation that is difficult to replicate through traditional instruction alone.
The Importance of Psychosocial Normality
Reflecting on his childhood, Schoenbauer emphasizes a crucial aspect of pediatric care that is often overlooked in clinical settings: the need for "normality." He recalls that while adults were often overly cautious or "gentle" with him, his most cherished memories involve friends who treated him as an equal. Playing video games with peers provided a rare space where his physical limitations were irrelevant.
This observation aligns with modern pediatric oncology protocols that stress the importance of maintaining social connections and age-appropriate activities for children undergoing treatment. Research suggests that children who maintain a sense of "normalcy" during cancer treatment experience better long-term psychosocial outcomes and lower rates of post-traumatic stress disorder (PTSD). Schoenbauer’s advice to those supporting children with cancer is simple: provide them with opportunities to be a regular kid.
Broader Implications and Future Outlook
The story of Luke Schoenbauer is more than a narrative of individual triumph; it reflects broader trends in oncology and rehabilitative medicine. The five-year survival rate for localized osteosarcoma has increased significantly over the last several decades, now hovering around 70% due to advancements in multi-agent chemotherapy and surgical techniques. However, the focus of the medical community is increasingly shifting toward "survivorship"—ensuring that survivors like Schoenbauer not only live but thrive with a high quality of life.

As Schoenbauer prepares to receive his white coat and enter the workforce, he represents a new generation of healthcare providers who bring deep personal empathy to evidence-based practice. His career will likely involve helping patients navigate the same frustrations he faced—ill-fitting prosthetics, the physical toll of recovery, and the emotional burden of a life-changing diagnosis.
In the field of physical therapy, the integration of practitioners with personal experience in disability is gaining recognition as a vital asset. It challenges the traditional "top-down" model of care, replacing it with a collaborative partnership between provider and patient. For Schoenbauer, his prosthetic leg is not just a tool for mobility; it is a bridge to his patients and a badge of a hard-won expertise that no textbook can fully convey. As he prepares for his graduation in May, his journey serves as a powerful reminder that the most effective healers are often those who have walked the path of the patient themselves.

