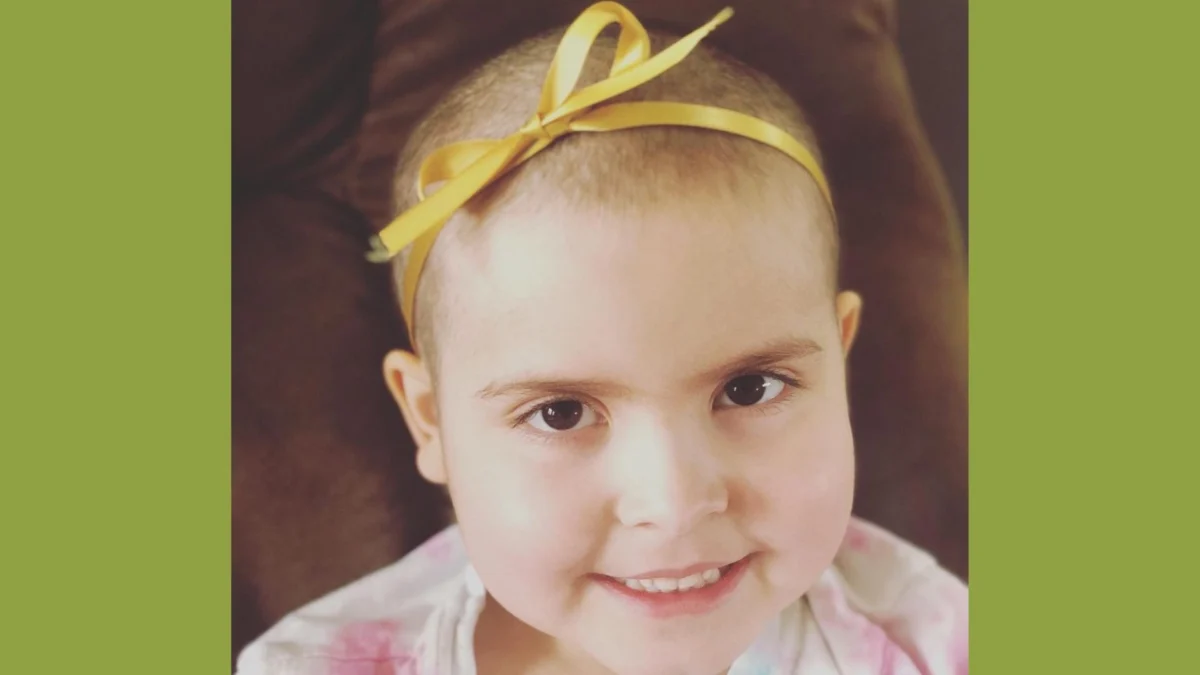
The transition from a healthy childhood to a life-altering medical crisis often begins with subtle, easily overlooked symptoms. For five-year-old Era and her parents, Cheri and Drew, the warning signs appeared as intermittent pain, a gradual loss of weight, and a persistent, ghostly pallor. It was the observation of a seasoned emergency room nurse, however, that first signaled the gravity of the situation. Cheri recalls the unspoken dread in the nurse’s expression—a look of professional recognition that preceded the formal delivery of life-changing news. Within hours, the family was informed that malignancies had been detected in Era’s bloodwork, a clinical term that Cheri had to translate into the devastating reality of cancer for her husband.
Era was diagnosed with acute lymphoblastic leukemia (ALL), a malignancy of the white blood cells that stands as the most common form of childhood cancer. While medical advancements have significantly improved the prognosis for ALL over the last several decades, the treatment remains a grueling, multi-year marathon involving intensive chemotherapy, frequent hospitalizations, and a suite of invasive procedures. For Era’s family, the diagnosis was compounded by a painful history; Drew’s cousin had previously succumbed to cancer as a teenager, casting a long shadow of fear over the family’s new reality.
The Clinical Reality of Acute Lymphoblastic Leukemia
Acute lymphoblastic leukemia is a fast-growing cancer of the lymphoid cells. In a healthy child, the bone marrow produces stem cells that mature into various types of blood cells. In a child with ALL, the marrow produces too many immature white blood cells, known as lymphoblasts, which fail to function correctly and crowd out healthy red blood cells and platelets. This leads to the symptoms Era exhibited: anemia (causing her extreme paleness), weight loss, and bone pain.
According to the American Cancer Society, ALL accounts for approximately three out of every four cases of childhood leukemia. While the five-year survival rate for children with ALL has risen to about 90%, the journey to remission is fraught with challenges. Treatment protocols are standardized but rigorous, typically divided into three main phases: induction, consolidation, and maintenance.

- Induction Therapy: The goal is to kill the leukemia cells in the blood and bone marrow to get the cancer into remission. This usually lasts a month and is the most intensive phase.
- Consolidation (Intensification): This phase aims to eliminate any remaining leukemia cells that may not be active but could cause a relapse.
- Maintenance Therapy: This is the longest phase, often lasting two to three years, intended to prevent the cancer from returning.
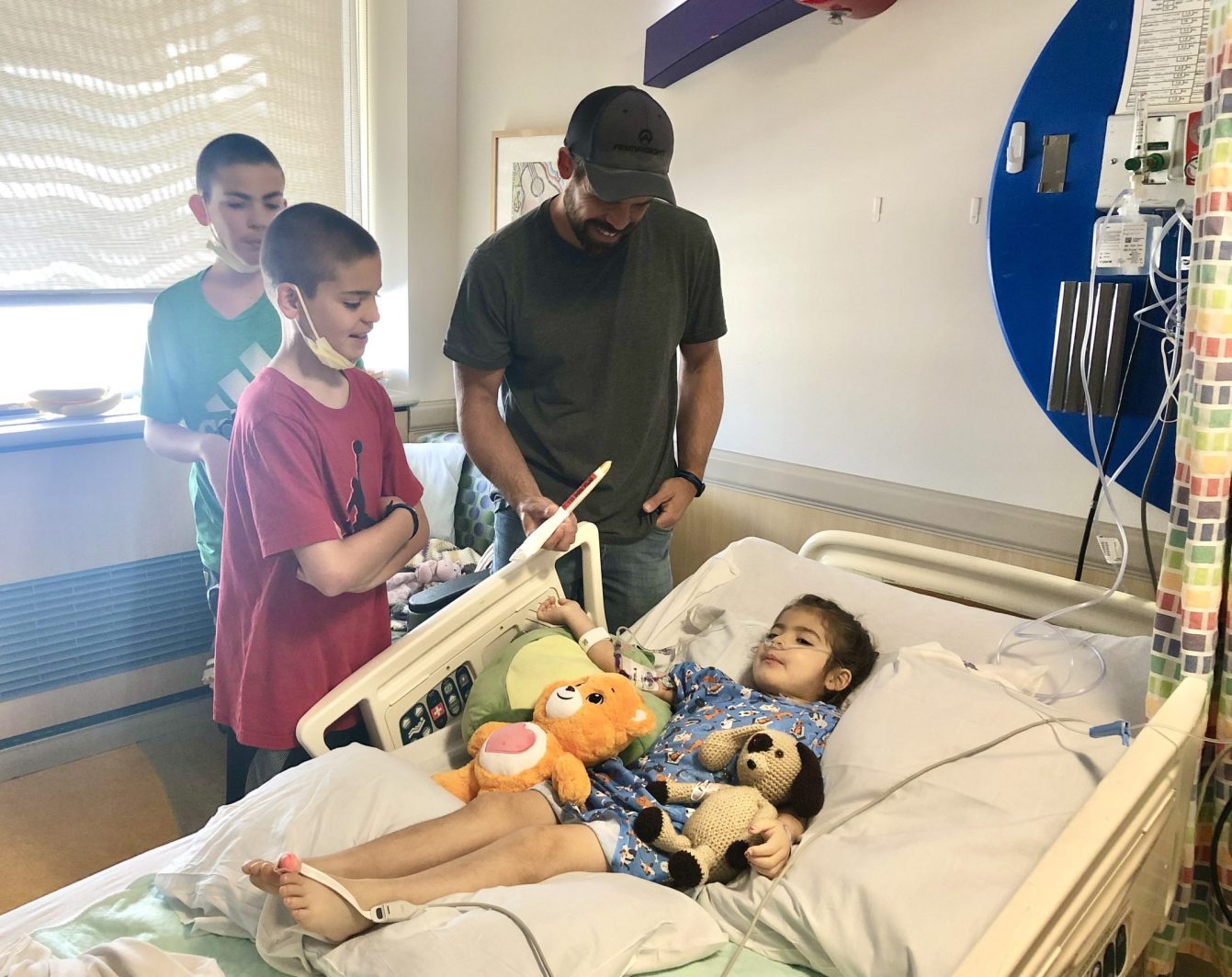
For Era, this meant her childhood was abruptly replaced by a schedule of lumbar punctures, blood draws, and chemotherapy cycles—a regimen that would test the resilience of even the strongest adult.
A Strategy of Resilience: The Families Psychological Approach
In the wake of the diagnosis, Cheri and Drew made a conscious decision to manage the emotional environment surrounding Era. From the confines of a hospital bathroom, they coordinated with extended family members, delivering the news while simultaneously issuing a mandate: they required a collective front of positivity. Cheri recognized early on that while she could not control the genetic mutations in her daughter’s blood or the toxicity of the life-saving medications, she could control the family’s psychological response.
"When this happens, everything is stripped away from you," Cheri noted, reflecting on the loss of autonomy that accompanies a pediatric cancer diagnosis. "You really have no choice but to do what the doctors recommend. But you can control how you approach it."
This "mindset-first" approach is increasingly recognized by pediatric psychologists as a vital component of patient care. By maintaining a sense of "silliness" and normalcy, the family aimed to mitigate the trauma of treatment. This strategy was not born of denial but of a calculated effort to preserve Era’s spirit during a period of physical devastation.
The Pediatric Coping Toolbox
Navigating the landscape of pediatric oncology requires more than just medical intervention; it requires a specialized set of tools to help a child process pain and fear. Era, like many children undergoing long-term treatment, developed a "coping toolbox" to manage the "pokes" and procedures that became her new normal. These strategies often involve:
- Child Life Specialists: Professionals trained to explain medical procedures in age-appropriate language and provide distraction during painful events.
- Medical Play: Using dolls or kits to allow the child to "perform" the procedures themselves, reclaiming a sense of agency.
- Distraction Techniques: Utilizing tablets, toys, or storytelling to divert attention during needle sticks or lumbar punctures.
- Positive Reinforcement: Rewards systems, such as "Beads of Courage," where children receive a specific bead for every milestone or procedure they endure.
These tools are essential because the psychological impact of childhood cancer can be long-lasting. Research indicates that survivors of childhood cancer are at a higher risk for post-traumatic stress disorder (PTSD) and anxiety later in life. By equipping Era with coping mechanisms early on, her family and medical team were working to safeguard her long-term mental health.
The Funding Gap: A Crisis in Pediatric Research
While Era’s personal battle is a story of individual resilience, it also highlights a systemic issue in the medical community: the staggering lack of funding for pediatric cancer research. Cheri’s frustration with the current state of treatment options is echoed by advocates nationwide. Despite the prevalence of childhood cancer, it remains significantly underfunded compared to adult cancers.
Data from the National Cancer Institute (NCI) and various advocacy groups show that only about 4% of federal funding for cancer research is specifically directed toward childhood cancers. This discrepancy has profound implications for the development of new therapies.
"I think people assume that new cancer treatments are being developed every year… that’s the case for adults," Cheri explained. "For kids, most of their treatment options are five or six times as old as they are."
The pharmaceutical industry also lacks a strong financial incentive to develop drugs for children. Because the "market" for pediatric cancer is smaller than that for adult cancers like lung or breast cancer, the return on investment for new pediatric drugs is often seen as insufficient. Consequently, children are often treated with "repurposed" adult drugs. Of the hundreds of cancer drugs approved by the FDA, fewer than 10 were developed specifically for pediatric use from the outset.

This reliance on older, more toxic therapies means that while more children are surviving, they are doing so at a high cost. Up to 95% of childhood cancer survivors will develop a significant health-related issue by the age of 45, including heart disease, secondary cancers, and cognitive impairments, all caused by the very treatments that saved their lives.
The Role of Private Philanthropy and Community Support
In the absence of robust federal and industrial funding, the burden of financing life-saving research has fallen largely on private charitable foundations and the families of patients themselves. Organizations such as the Children’s Cancer Research Fund (CCRF) play a critical role in bridging this gap. These foundations fund the "seed" research—innovative, high-risk, high-reward studies—that federal agencies are often hesitant to back.
For families like Era’s, the transition from being occasional donors to becoming active advocates is a common trajectory. Cheri admitted that before Era’s diagnosis, their family donated occasionally but didn’t fully grasp the urgency of the cause. "Now, we don’t get to stop thinking about it," she said.
The sustainability of pediatric cancer research depends on a shift in public perception. Advocates argue that the responsibility should not rest solely on the shoulders of traumatized families. Instead, it requires a concerted effort from the broader community to demand better funding and more modern treatment options for the youngest and most vulnerable patients.
Broader Implications and the Path Forward
The story of Era and her family is a microcosm of a larger national health challenge. As diagnostic tools improve, the medical community is getting better at identifying childhood cancers earlier. However, the development of "precision medicine"—treatments tailored to the genetic makeup of an individual’s tumor—is lagging in the pediatric sector due to the aforementioned funding constraints.

The path forward involves several key components:
- Legislative Advocacy: Pushing for acts like the STAR Act (Survival, Treatment, Access, and Research) and the RACE for Children Act, which aim to increase pediatric research and require companies to test adult cancer drugs in children.
- Increased Federal Allocation: Advocating for a larger slice of the NCI budget to be dedicated to pediatric-specific studies.
- Community Awareness: Educating the public on the "4% reality" to drive more consistent, year-round support for research foundations.
As Era continues her treatment, her family remains focused on the immediate goal of health and the broader goal of change. Their experience serves as a reminder that behind every statistic is a child whose future depends on the scientific advancements of today. For Cheri, the goal is simple: ensuring that the next family to walk into an emergency room doesn’t have to rely on decades-old medicine to save their child’s life.
The fight against childhood cancer is not a solitary one; it is a collective endeavor that requires the sustained attention and resources of society at large. Through a combination of medical innovation, psychological support, and aggressive advocacy, the hope is that one day, the diagnosis of "malignancies in the bloodwork" will no longer be a sentence of years-long trauma, but a manageable hurdle on the path to a long and healthy life.