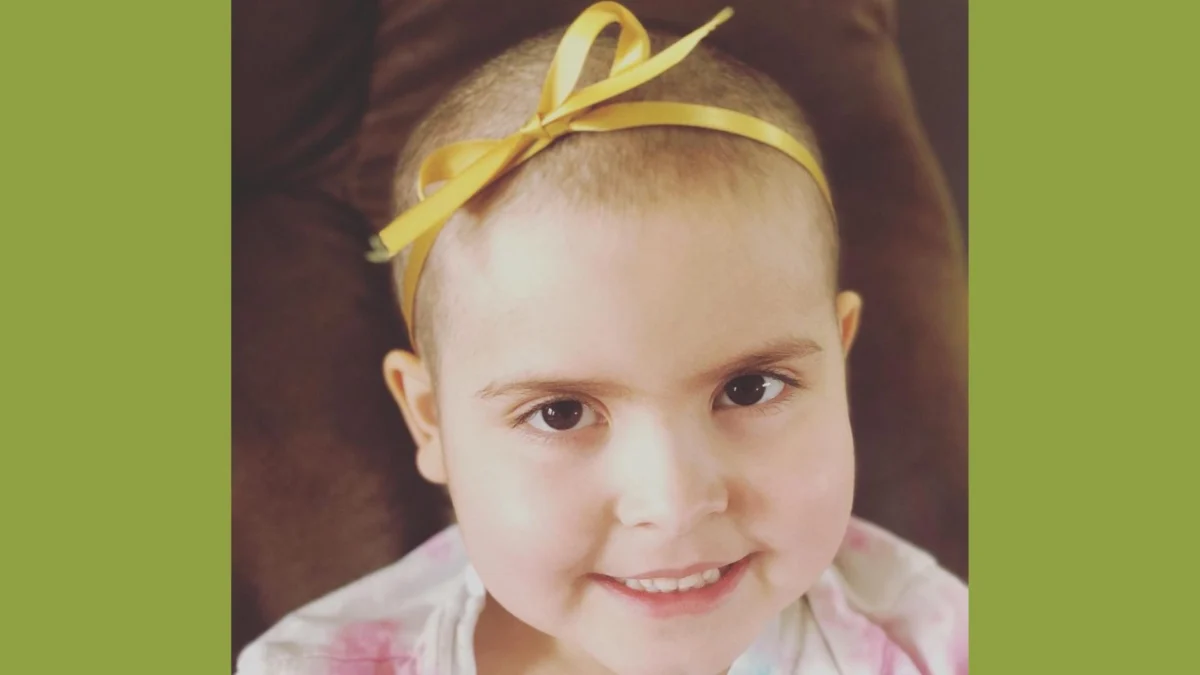
The diagnostic journey for families navigating pediatric cancer often begins not with a definitive test, but with a series of subtle, unsettling physical changes that culminate in a life-altering moment within the sterile walls of an emergency department. For Cheri and Drew Ham, the reality of this transition crystallized through the expression of an emergency room nurse examining their five-year-old daughter, Era. The nurse’s countenance, described by Cheri as a silent admission of impending bad news, preceded a formal diagnosis that would thrust the family into the complex world of pediatric oncology. Era had exhibited intermittent pain for several months, accompanied by noticeable weight loss and a striking pallor that extended even to her earlobes—a clinical sign of severe anemia often associated with hematologic malignancies.
Within hours of their arrival at the hospital, medical professionals delivered the results of Era’s bloodwork, identifying the presence of malignancies. The terminology, while clinical, carried a devastating weight. When Drew questioned the meaning of "malignancies in the bloodwork," the reality was distilled into a single word: cancer. This specific diagnosis was identified as Acute Lymphoblastic Leukemia (ALL), a cancer of the blood and bone marrow that stands as the most common form of childhood malignancy. While ALL has seen significant improvements in survival rates over the last half-century, the treatment regimen remains one of the most grueling in pediatric medicine, typically requiring multiple phases of chemotherapy spanning two to three years.
The Clinical Profile of Acute Lymphoblastic Leukemia
Acute Lymphoblastic Leukemia is characterized by the overproduction of immature white blood cells, known as lymphoblasts. These cancerous cells crowd out healthy red blood cells, white blood cells, and platelets in the bone marrow, leading to the symptoms Era experienced: fatigue and pallor from anemia, bone pain from marrow overcrowding, and potential bruising or weight loss. According to data from the American Cancer Society, ALL accounts for approximately half of all leukemia cases in children and nearly one-third of all pediatric cancer diagnoses.

The standard of care for ALL is divided into several phases: induction, consolidation (or intensification), and maintenance. The induction phase aims to achieve complete remission by eliminating the bulk of leukemia cells. This is followed by consolidation to target any residual disease, and finally, a long-term maintenance phase to prevent relapse. For a five-year-old child, this means years of intravenous infusions, oral medications, and invasive procedures such as lumbar punctures—often referred to as spinal taps—to ensure the cancer has not spread to the central nervous system.
Psychological Management and the Coping Toolbox
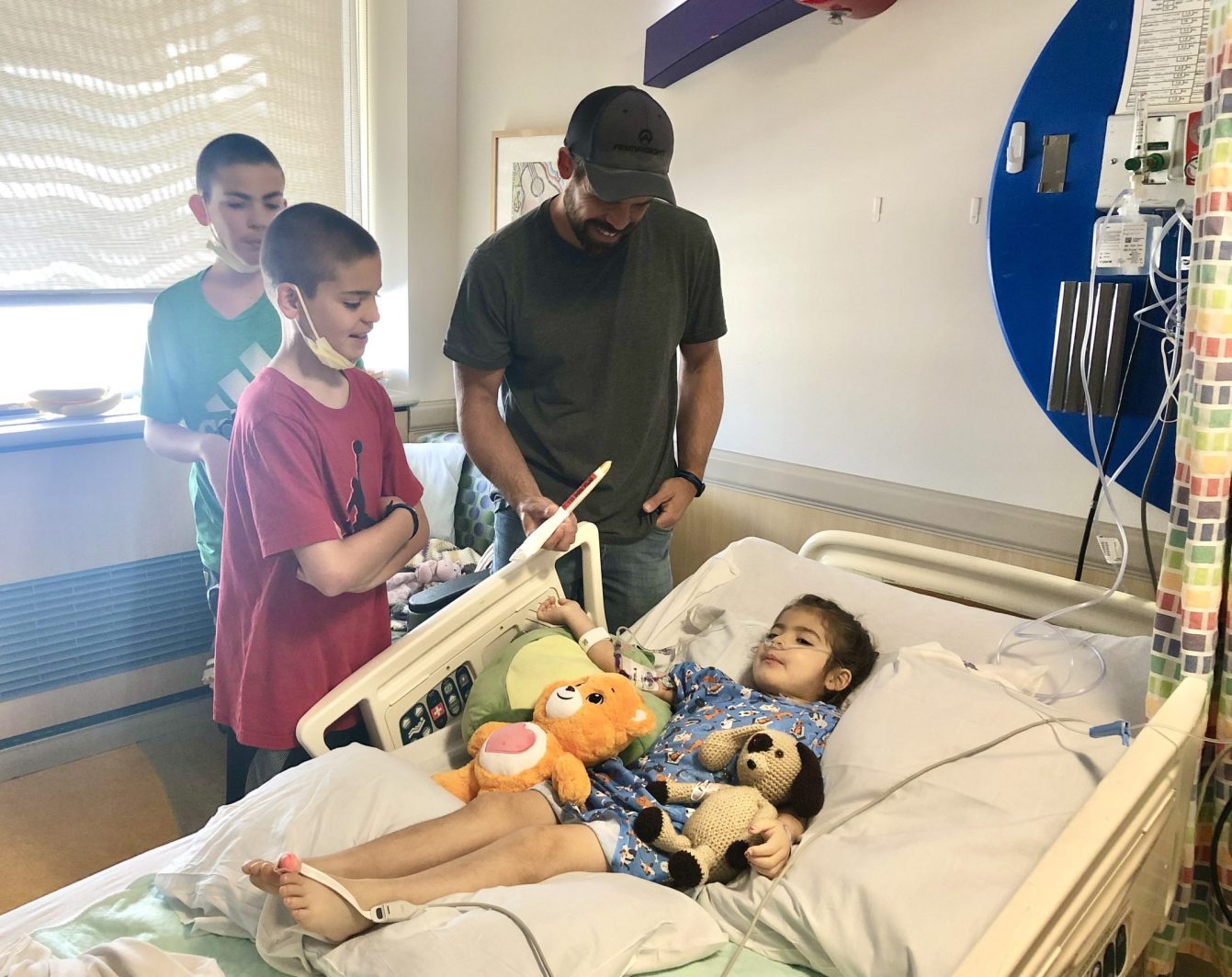
The Ham family’s response to the diagnosis highlights a critical aspect of pediatric cancer care: the psychological management of both the patient and the support system. Cheri Ham adopted a strategy of radical positivity, a choice made to mitigate the fear and negativity that often permeate a hospital environment. By maintaining a sense of normalcy and "silliness" even within the oncology ward, the family sought to preserve Era’s childhood despite the clinical demands of her condition. This approach is supported by various studies in pediatric psychology, which suggest that a child’s ability to cope with chronic illness is heavily influenced by the emotional regulation and "modeling" provided by their primary caregivers.
To navigate the physical trauma of treatment, Era developed what the family calls a "coping toolbox." In the absence of specialized pediatric medications that minimize side effects, children must often rely on behavioral interventions to manage the pain of "pokes" and the discomfort of chemotherapy. Standard pediatric coping tools often include:
- Distraction Therapy: Utilizing tablets, books, or toys to redirect the child’s focus during needle sticks or port accesses.
- Topical Anesthetics: The use of lidocaine creams (often called "magic cream" by young patients) to numb the skin prior to injections.
- Child Life Specialists: Professional interventionists who use age-appropriate play to explain medical procedures, thereby reducing the "fear of the unknown."
- Positive Reinforcement Systems: "Bravery beads" or sticker charts that allow children to visualize their progress and commemorate their courage through each procedure.
The Disparity in Pediatric Research and Development
A central theme in the Ham family’s experience is the frustration regarding the lack of innovation in pediatric cancer therapeutics. Cheri Ham noted that while the public often assumes cancer research is a monolithic field where all patients benefit from cutting-edge breakthroughs, the reality for pediatric patients is far different. There is a systemic "funding gap" that leaves children with treatment options that are often decades old.
Statistical analysis of oncology drug development reveals a stark contrast between adult and pediatric care. Historically, less than 10% of all cancer drugs have been designed specifically for children. While the pharmaceutical industry has produced hundreds of targeted therapies and immunotherapies for adult cancers—such as lung, breast, and prostate cancer—pediatric oncology remains largely reliant on "repurposed" adult chemotherapy drugs. These medications, while effective at killing cancer cells, are often highly toxic to developing bodies, leading to significant long-term health complications for survivors.
The National Cancer Institute (NCI) allocates approximately 4% of its annual budget specifically to childhood cancer research. This figure has long been a point of contention for advocacy groups, who argue that the unique biological makeup of pediatric tumors requires dedicated, well-funded research pathways. Because pediatric cancers are biologically distinct from adult cancers—often driven by developmental mutations rather than environmental factors or aging—they require a different therapeutic approach.
The Economic and Social Burden on Families
The burden of addressing this research gap often falls on the families who are already navigating the trauma of the disease. Charitable foundations, such as the Children’s Cancer Research Fund, provide over half of the funding for pediatric cancer research in the United States. These organizations are frequently fueled by "legacy" families—those who have either lost a child to cancer or whose children are in survivorship.
The Ham family’s transition from casual donors to active advocates underscores the isolation many families feel when the initial wave of community support wanes. Long-term treatment for ALL requires a sustained commitment that can strain a family’s financial stability and emotional reserves. The "trauma of treatment" does not end with the final dose of chemotherapy; it continues through years of follow-up appointments and the constant monitoring for late-onset side effects, which can include heart disease, secondary cancers, and cognitive impairments.

Implications for Public Policy and Community Support
The story of Era Ham serves as a microcosmic view of a larger public health challenge. To advance the field of pediatric oncology, experts suggest that several systemic changes are necessary:
- Increased Federal Funding: Advocacy for a higher percentage of the NCI budget to be earmarked for pediatric-specific trials.
- Incentivizing Pediatric Drug Development: Strengthening legislation, such as the RACE for Children Act, which requires drug companies to test new adult cancer drugs in children if the molecular targets are relevant to pediatric tumors.
- Philanthropic Sustainability: Moving beyond "one-time" donations toward sustained community support for research foundations.
The Ham family’s resolve to maintain a positive mindset is a testament to the resilience of the human spirit, but as Cheri Ham points out, mindset alone cannot cure cancer. It requires the scientific community to have the resources necessary to develop safer, more effective treatments. The reliance on decades-old chemotherapy protocols is a reminder that while survival rates have improved, the quality of life during and after treatment remains a critical area for improvement.
Conclusion: A Call for Collective Action
Era Ham’s journey from a pale, pained five-year-old to a "fighter" in the oncology ward is a narrative shared by thousands of families every year. The "malignancies in the bloodwork" that shattered Drew Ham’s world are a call to action for a broader societal commitment to pediatric health. The current landscape, where families must take turns calling relatives from hospital bathrooms to deliver devastating news, is compounded by the knowledge that their children are being treated with medications that were developed before they were born.
The Ham family’s experience highlights that pediatric cancer is not just a medical crisis, but a social and economic one. It requires a collective effort from the medical community, legislators, and the public to ensure that the "coping toolbox" of the future includes not just stickers and distraction, but precision medicines designed specifically for the smallest and most vulnerable patients. By supporting research organizations and advocating for policy changes, the community can ensure that families like Era’s do not have to fight the battle against cancer and the battle against a lack of funding simultaneously. The goal remains a future where a diagnosis of ALL is met not just with resolve and "silliness," but with the certainty of modern, targeted, and gentle cures.