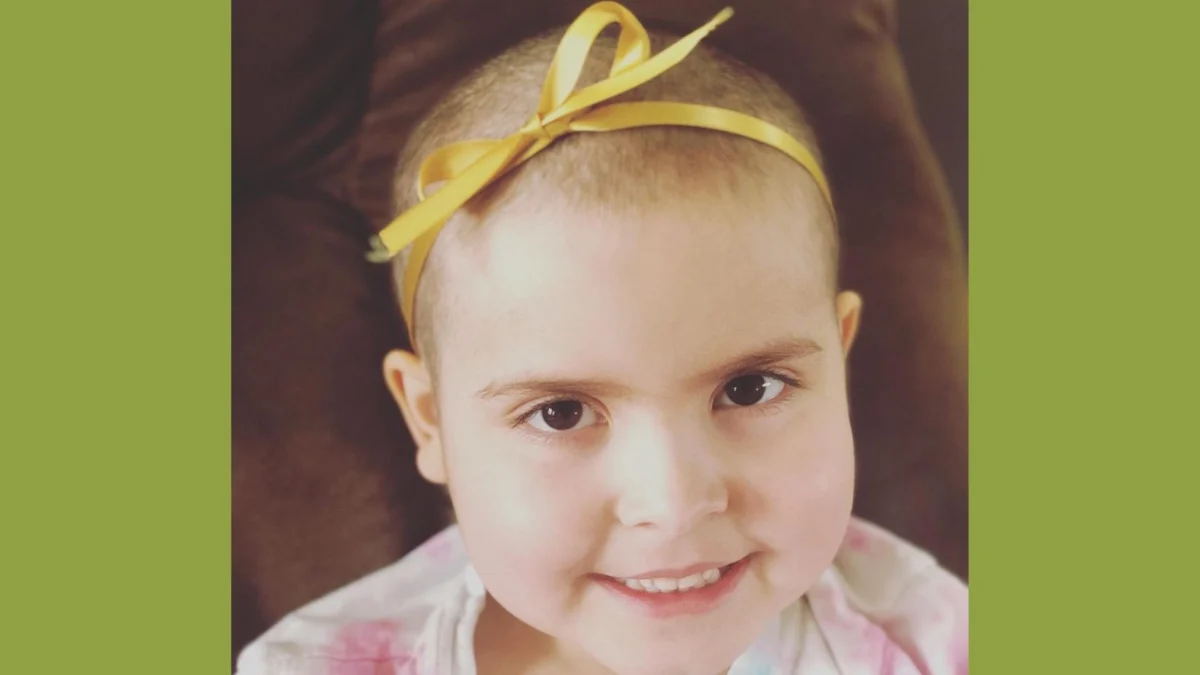
The transition from a routine medical concern to a life-altering diagnosis often occurs in the quiet, sterile atmosphere of an emergency department, marked not by a sudden event, but by the subtle shift in a clinician’s demeanor. For Cheri and Drew, the parents of five-year-old Era, that shift manifested in the expression of an emergency room nurse who examined their daughter following months of intermittent physical distress. Era had been plagued by recurring pain, significant weight loss, and a striking pallor that had reached even her earlobes—symptoms that, in retrospect, served as the clinical heralds of a systemic failure within her young body. Within hours of their arrival, the clinical team returned with bloodwork results that confirmed the presence of malignancies, a term that necessitated a blunt translation for the grieving parents: their daughter had cancer.
Era was subsequently diagnosed with Acute Lymphoblastic Leukemia (ALL), a malignancy of the blood and bone marrow that stands as the most common form of childhood cancer. While advancements in pediatric oncology have significantly improved survival rates for ALL over the last half-century, the diagnosis remains a grueling ordeal for the patient and a traumatic upheaval for the family unit. For Era’s family, the news was compounded by a haunting familial history; Drew’s cousin had previously succumbed to cancer as a teenager, casting a long shadow of apprehension over the prognosis. This personal history underscores the visceral fear many families face when entering the world of pediatric oncology—a world where the stakes are absolute and the protocols are demanding.
The Clinical Landscape of Acute Lymphoblastic Leukemia
Acute Lymphoblastic Leukemia is characterized by the overproduction of immature white blood cells, known as lymphoblasts. In a healthy body, these cells develop into mature lymphocytes that form the backbone of the immune system. In a patient with ALL, however, these abnormal cells multiply rapidly, crowding out healthy red blood cells, white blood cells, and platelets. This leads to the classic symptoms observed in Era: anemia (causing paleness), increased susceptibility to infection, and easy bruising or bone pain.

The standard of care for ALL is one of the most intensive regimens in modern medicine. Treatment typically spans two to three years and is divided into several phases: induction, consolidation, and maintenance. Induction therapy aims to kill the leukemia cells in the blood and bone marrow to put the cancer into remission. This is followed by consolidation therapy to eliminate any remaining undetected cells, and finally, a long-term maintenance phase to prevent recurrence. For a five-year-old child, this means years of chemotherapy, frequent lumbar punctures to protect the central nervous system, and a litany of medications that carry significant side effects.
A Chronology of Diagnosis and the Psychology of Resilience
The timeline of Era’s diagnosis followed a pattern familiar to many pediatric oncology families. What began as "on-again, off-again" pain was initially difficult to pin down, a common occurrence in pediatric cases where symptoms can mimic growing pains or minor viral infections. However, the progression of physical wasting and the loss of healthy skin tone eventually signaled a deeper systemic issue. The speed with which the emergency room visit escalated into an oncology admission highlights the aggressive nature of childhood leukemias, which require immediate intervention to prevent rapid deterioration.
In the wake of the diagnosis, Cheri and Drew adopted a strategy of "radical positivity," a psychological defense mechanism often utilized by parents to shield their children from the secondary trauma of a medical crisis. From the confines of a hospital bathroom, the couple coordinated with their extended family, demanding a unified front of strength and optimism. Cheri’s insistence that Era should not "feel any negativity or fear" represents a common parental effort to maintain a sense of normalcy in an environment that is fundamentally abnormal. This approach, while born of necessity, highlights the immense emotional labor required of caregivers who must manage their own grief while simultaneously serving as the primary emotional anchors for their children and other siblings.
The Funding Disparity in Pediatric Cancer Research
Despite the prevalence of childhood cancer, a significant gap exists between the public perception of research progress and the reality of clinical funding. Cheri’s observation that "most of their treatment options are five or six times as old as they are" is supported by current pharmacological data. While adult oncology has seen a revolution in targeted therapies and immunotherapies over the last two decades, pediatric oncology continues to rely heavily on cytotoxic chemotherapy drugs developed in the mid-20th century.
Data from the National Cancer Institute (NCI) and various advocacy groups reveal a stark disparity in resource allocation. It is frequently cited that only approximately 4% of federal funding for cancer research is dedicated specifically to pediatric cancers. The pharmaceutical industry, driven by market size and return on investment, often prioritizes adult cancers—such as lung, breast, and prostate cancer—which affect hundreds of thousands of individuals annually. Because pediatric cancers are considered "rare" in a statistical sense, there is less commercial incentive to develop new, age-specific drugs.
Of the hundreds of oncology drugs approved by the FDA, fewer than ten were developed specifically for pediatric use from the outset. Most medications used to treat children like Era were originally designed for adults and are later "repurposed" for children through dose adjustments. This lack of specific innovation means that children are often subjected to treatments that are unnecessarily toxic to their developing bodies, leading to long-term health complications known as "late effects," which can include heart disease, secondary cancers, and cognitive impairments.
The Role of the Coping Toolbox in Pediatric Care
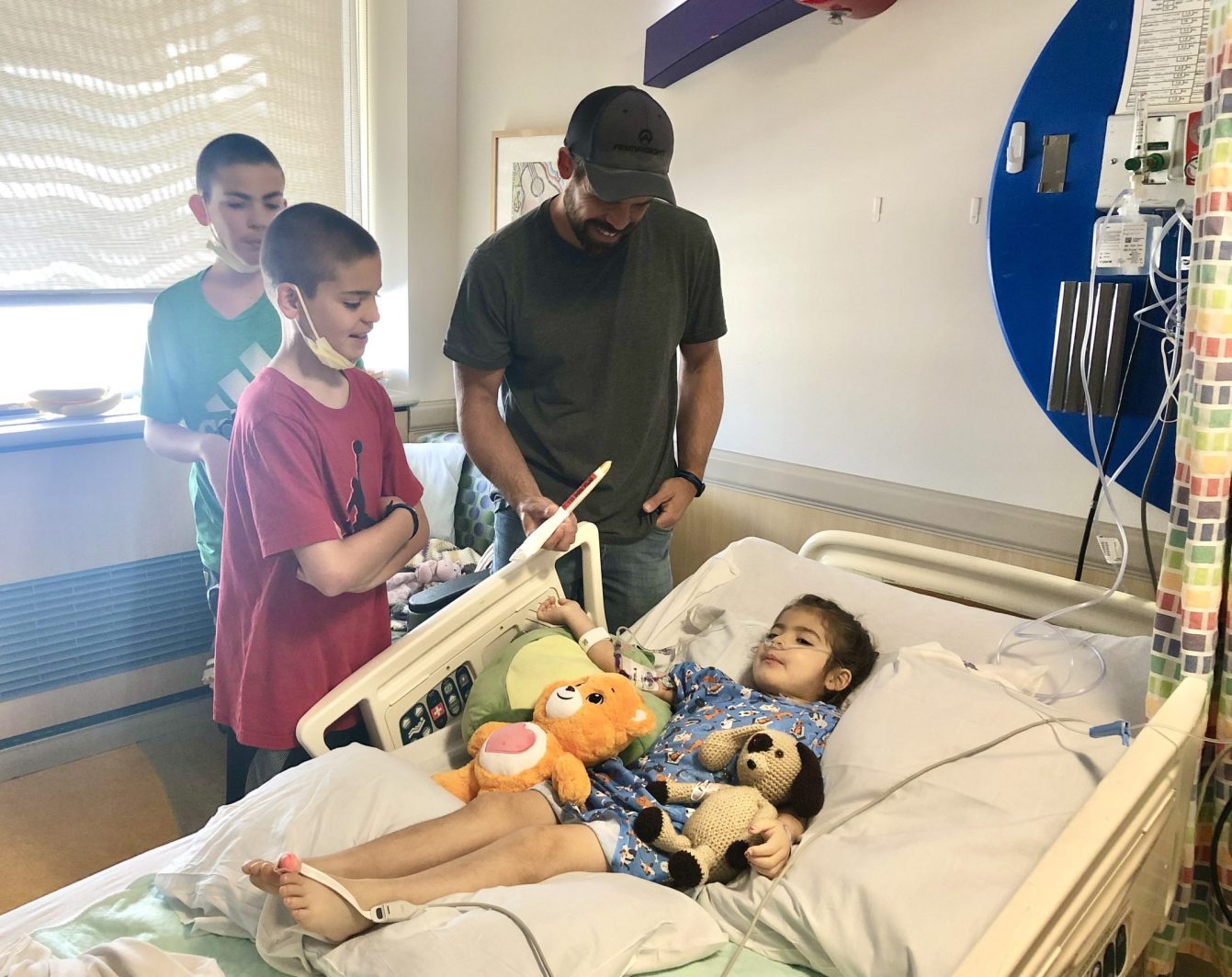
For a young child, the hospital environment is a place of inherent trauma. Procedures that are routine for clinicians—such as blood draws, lumbar punctures, and the administration of foul-tasting oral medications—are perceived as assaults by a five-year-old. To navigate this, pediatric hospitals and families develop "coping toolboxes." These are not merely physical boxes of toys, but a set of psychological and sensory strategies designed to give the child a sense of agency in a situation where they have none.
Era’s experience involved developing specific strategies for every "poke" and procedure. These toolboxes often include distraction techniques, such as using virtual reality or iPads, the use of topical numbing creams (like EMLA) to reduce the pain of needle sticks, and "bravery beads" or other reward systems that track the child’s progress through their treatment milestones. These interventions are critical because they help prevent the development of medical PTSD, a condition that can affect pediatric survivors well into adulthood.

Broader Implications and the Necessity of Community Support
The burden of changing the landscape of pediatric cancer research currently falls disproportionately on the families of those affected. As Cheri noted, over half of all funds raised for childhood cancer research are generated by private charitable foundations and families who are themselves still reeling from the trauma of treatment. This reliance on "grassroots" funding is a testament to the resilience of the community but also a critique of the systemic neglect of pediatric health priorities.
The implications of this funding gap extend beyond the immediate survival of the child. Because current treatments are so harsh, the "cost" of a cure is often a lifetime of chronic health issues. Advancing research is not just about increasing survival rates—which are already high for certain types of ALL—but about developing "kinder" treatments that eliminate the cancer without destroying the patient’s long-term quality of life.
The call to action from families like Era’s is a plea for sustainable, community-wide support. Charitable organizations like the Children’s Cancer Research Fund (CCRF) serve as vital conduits for this support, funding the early-stage "seed" research that federal agencies and pharmaceutical companies are often unwilling to risk. By investing in these foundations, the public helps bridge the gap between old, toxic protocols and the next generation of precision medicine.
Conclusion
The story of Era is a microcosm of a larger national crisis in pediatric healthcare. While her family continues to fight for her health with a determined mindset and a "coping toolbox," they are operating within a system that has historically underfunded the very innovations they need most. The resolve of parents to remain "silly" and "positive" in the face of malignancy is a powerful display of the human spirit, but it is not a substitute for clinical progress.

To ensure that future five-year-olds do not have to rely on decades-old medications, a fundamental shift in how society prioritizes and funds pediatric oncology is required. The transition from a "family-only" struggle to a collective community mission is the only way to ensure that the progress seen in adult cancer care is mirrored in the pediatric wards. As Era continues her journey through the rigorous phases of ALL treatment, her story serves as a reminder that while survival is the goal, the ultimate objective must be a future where childhood cancer can be treated with the safety, precision, and dignity that every child deserves.