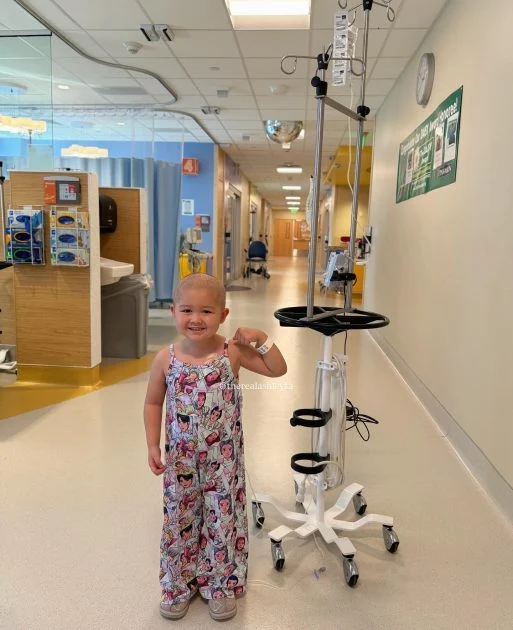
The intersection of maternal intuition and clinical diagnostics often forms the first line of defense in pediatric oncology, a reality exemplified by the recent appointment of four-year-old Rylee as a 2026 Ambassador for the American Childhood Cancer Organization (ACCO). Rylee, who is currently undergoing treatment for Acute Lymphoblastic Leukemia (ALL), represents a demographic of pediatric patients whose diagnoses are frequently preceded by a period of intensive parental advocacy. Her case highlights not only the biological challenges of childhood leukemia but also the systemic hurdles within the healthcare system that parents must navigate to secure timely interventions.
The diagnostic journey for Rylee began with a series of non-specific symptoms that initially eluded definitive clinical categorization. According to accounts provided by her mother, Ashley, the family sought medical attention multiple times as Rylee exhibited a fluctuating array of symptoms, including persistent fevers, chills, body aches, a swollen eye, lymphadenopathy, unexplained bruising, and joint pain. Despite repeated visits to urgent care facilities and emergency departments, initial clinical assessments attributed these signs to minor infections or seasonal allergies. This period of diagnostic uncertainty is a documented phenomenon in pediatric oncology, where the early signs of malignancy can often mimic common childhood illnesses, necessitating a high degree of clinical suspicion and persistent parental reporting.
On August 6, the trajectory of Rylee’s care shifted when Ashley insisted on a comprehensive blood panel following a lack of resolution in her daughter’s condition. The results, delivered at 5:00 p.m. that evening, confirmed a diagnosis of leukemia. The timing of the diagnosis introduced additional domestic complexity, as Rylee’s father, Jacob, was serving on an overseas military deployment at the time. This left Ashley to manage the immediate medical crisis and the subsequent emergency ambulance transport to a specialized pediatric facility in Denver, Colorado, independently.
Clinical Intervention and the First Phase of Treatment
Upon arrival at the tertiary care center in Denver, Rylee underwent an intensive induction phase of treatment. Within the first week of her hospitalization, several critical procedures were performed to stabilize her condition and begin the eradication of malignant cells. These included the surgical placement of a chemo-port—a central venous access device used to deliver medication and draw blood—and a bone marrow biopsy to further characterize the leukemia.
Furthermore, Rylee received a lumbar puncture, a procedure essential for both diagnostic staging and prophylactic treatment. During this procedure, chemotherapy agents were administered directly into the spinal fluid to prevent the spread of leukemia cells to the central nervous system, a common complication in ALL patients. The initial week of treatment also required three blood transfusions and two platelet transfusions to address the hematological deficiencies caused by both the disease and the aggressive start of chemotherapy.
By early September, clinical evaluations indicated that Rylee had achieved a state of remission. In oncology, remission signifies that the signs and symptoms of cancer have decreased or disappeared, though it does not necessarily mean the patient is cured. For pediatric ALL, the standard of care involves a multi-year treatment plan to ensure that residual microscopic disease is eliminated. Rylee’s prescribed treatment protocol is scheduled to continue through October 2027, highlighting the long-term commitment required for pediatric cancer survivors and their families.
Innovative Therapeutics: The Role of Blinatumomab
In October, Rylee transitioned to a newer class of immunotherapy known as Blinatumomab, often referred to by the clinical shorthand "Blina." Blinatumomab is a bispecific T-cell engager (BiTE) antibody that works by directing the body’s own immune system, specifically T-cells, to target and destroy leukemia cells expressing the CD19 protein.
Unlike traditional chemotherapy, which is often administered in high-dose bursts at a clinic, Blinatumomab requires a continuous intravenous infusion over a 28-day cycle. To maintain a semblance of normalcy and mobility, pediatric patients like Rylee utilize a portable infusion pump. Rylee carries her medication in a specialized "superhero" backpack, allowing her to receive life-saving treatment while engaging in the typical activities of a four-year-old, such as riding a bike or playing with her siblings. This method of delivery represents a significant advancement in pediatric oncology, focusing on maintaining the patient’s quality of life during extended treatment periods.
Supporting Data: The Landscape of Pediatric Leukemia
Acute Lymphoblastic Leukemia remains the most common form of childhood cancer, accounting for approximately 25% of all cancer diagnoses in children under the age of 15. According to the National Cancer Institute, while the five-year survival rate for pediatric ALL has seen a dramatic increase from less than 10% in the 1960s to approximately 90% today, the intensity of the treatment remains a significant burden on the developing physiology of the child.
Data from the American Cancer Society suggests that approximately 3,000 children and adolescents are diagnosed with ALL each year in the United States. While the prognosis is generally favorable compared to other malignancies, the long-term effects of chemotherapy and radiation—including potential impacts on cognitive development, cardiac health, and secondary malignancies—necessitate continuous monitoring. Organizations like the ACCO emphasize that "remission" is merely the beginning of a long road of survivorship that requires robust psychological and social support systems.
The ACCO Ambassador Program and Medical Play
As a 2026 ACCO Ambassador, Rylee serves as a public face for the thousands of children battling cancer. The ACCO, founded in 1970, is one of the oldest and largest grassroots childhood cancer organizations in the United States. Their Ambassador program aims to personalize the statistics of childhood cancer, providing a platform for families to share their stories and advocate for increased research funding and improved patient resources.
One of the primary tools provided by the ACCO to assist children in processing their medical experiences is the "Medical Play Kit." These kits are designed to help children understand the complex procedures they undergo by allowing them to engage with medical equipment in a non-threatening, play-based environment. Rylee’s engagement with these resources—documented in her "unboxing" videos where she expresses an interest in "becoming a doctor"—illustrates the psychological importance of agency. By "treating" her dolls or mimicking the actions of her healthcare providers, she transitions from a passive recipient of care to an active participant in her own healing process.
Implications for Patient Advocacy and Military Families
Rylee’s story brings to light two significant socio-medical issues: the necessity of parental advocacy and the unique stressors faced by military families during medical crises. Ashley’s directive to other parents—to "trust your gut" even when faced with clinical dismissal—resonates within the patient advocacy community. It underscores a growing recognition of the "parental intuition" factor in pediatric diagnostics, where a primary caregiver’s intimate knowledge of a child’s baseline behavior can be a critical diagnostic tool.
Furthermore, the deployment of Rylee’s father during her diagnosis highlights the challenges faced by the approximately 1.6 million "military children" in the United States. When a service member is deployed, the remaining parent often lacks the immediate physical and emotional support of their partner, complicating the logistics of long-term medical treatment. Rylee’s case has garnered attention for the resilience required by military families who must balance the demands of national service with the acute needs of a critically ill child.
Future Outlook and Continuing Care
The road ahead for Rylee is defined by a rigorous schedule of maintenance therapy that will span the next three years. This phase of treatment is designed to prevent relapse, which is most likely to occur within the first few years following the initial diagnosis. During this time, Rylee will continue to be monitored for minimal residual disease (MRD), a key prognostic indicator in ALL.
The broader implications of her journey as an ACCO Ambassador involve a call to action for increased federal funding for pediatric cancer research. Currently, only a small fraction of the National Cancer Institute’s budget is dedicated specifically to childhood cancers. Advocates argue that because children’s bodies are still developing, they require different therapeutic approaches than adults—approaches that are often less profitable for pharmaceutical companies to develop independently.
As Rylee continues her treatment through 2027, her role as an ambassador will involve participating in awareness campaigns and fundraising efforts. These initiatives are vital for the continued provision of free resources, such as the Medical Play Kits and peer support programs, which the ACCO provides to families at no cost. Her journey remains a testament to the efficacy of modern pediatric protocols and the indispensable role of persistent maternal advocacy in the face of medical adversity.