The American Cancer Society’s Cancer Statistics 2026 report unveils a compelling narrative of scientific triumph, particularly driven by advancements in immunotherapy and targeted treatments, which are now extending lives once considered beyond hope. This landmark report, a critical barometer of the nation’s battle against cancer, highlights an unprecedented milestone: the five-year relative survival rate for all cancers in the United States has reached a historic 70% during the period of 2015–2021. This figure marks a profound leap from a mere 49% in the mid-1970s, underscoring decades of relentless research and clinical innovation. Perhaps most profoundly, the report emphasizes dramatic gains in survival for advanced, metastatic cancers, a category that was, until recently, often deemed untreatable.
A Half-Century of Progress: A Chronology of Hope
The journey from a 49% survival rate in the mid-1970s to today’s 70% is not merely a statistical improvement; it represents a fundamental shift in the paradigm of cancer care. In the 1970s, cancer treatment primarily revolved around surgery, radiation therapy, and rudimentary chemotherapy. While these methods offered hope for some, particularly those with localized disease, options for advanced or metastatic cancers were severely limited, often resulting in grim prognoses. The ensuing decades witnessed incremental but significant progress. The 1980s and 1990s brought improved surgical techniques, more precise radiation delivery, and the development of new chemotherapy agents, albeit often accompanied by considerable side effects. Public health campaigns also began to gain traction, leading to increased awareness of risk factors and the importance of early detection through screenings.
The early 2000s marked the dawn of a new era with the emergence of targeted therapies. These drugs, unlike traditional chemotherapy, are designed to interfere with specific molecules involved in the growth, progression, and spread of cancer cells, thereby minimizing damage to healthy cells. The success of imatinib in chronic myeloid leukemia in 2001 was a harbinger of this new precision medicine approach, revolutionizing treatment for several cancer types.
However, the most transformative shift documented in the Cancer Statistics 2026 report is undoubtedly the rise of immunotherapy. While the concept of harnessing the body’s own immune system to fight cancer has been explored for over a century, it was only in the last two decades that groundbreaking discoveries translated into clinically effective treatments. Key milestones include the identification of immune checkpoints like CTLA-4 and PD-1 in the late 1990s and early 2000s. The subsequent development and approval of immune checkpoint inhibitors, such as ipilimumab (targeting CTLA-4) in 2011 and nivolumab and pembrolizumab (targeting PD-1) in 2014, fundamentally reshaped the treatment landscape for a growing number of cancers, including melanoma, lung cancer, and kidney cancer. These therapies have demonstrated remarkable and often durable responses, even in patients with advanced disease, effectively "rewriting survival curves" that had long been stagnant. The substantial philanthropic funding from organizations like the Cancer Research Institute (CRI) and governmental investment through the National Cancer Institute (NCI) in foundational immunology research played a crucial role in making these breakthroughs a reality.
The Current Cancer Burden: A Detailed Snapshot

Despite these remarkable strides, cancer remains a formidable public health challenge in the United States. The Cancer Statistics 2026 report projects an estimated 2.1 million Americans will be diagnosed with cancer in the coming year, leading to approximately 626,000 deaths. This translates to a staggering daily toll of about 5,800 new cases and 1,720 deaths, underscoring the pervasive impact of the disease across the nation.
Cancer maintains its position as the second leading cause of death overall in the U.S. However, its demographic impact is even more pronounced within specific age groups. For men aged 60–79 and women aged 40–79, cancer tragically stands as the leading cause of mortality. This highlights the critical need for continued vigilance in screening, prevention, and treatment strategies tailored to these vulnerable populations.
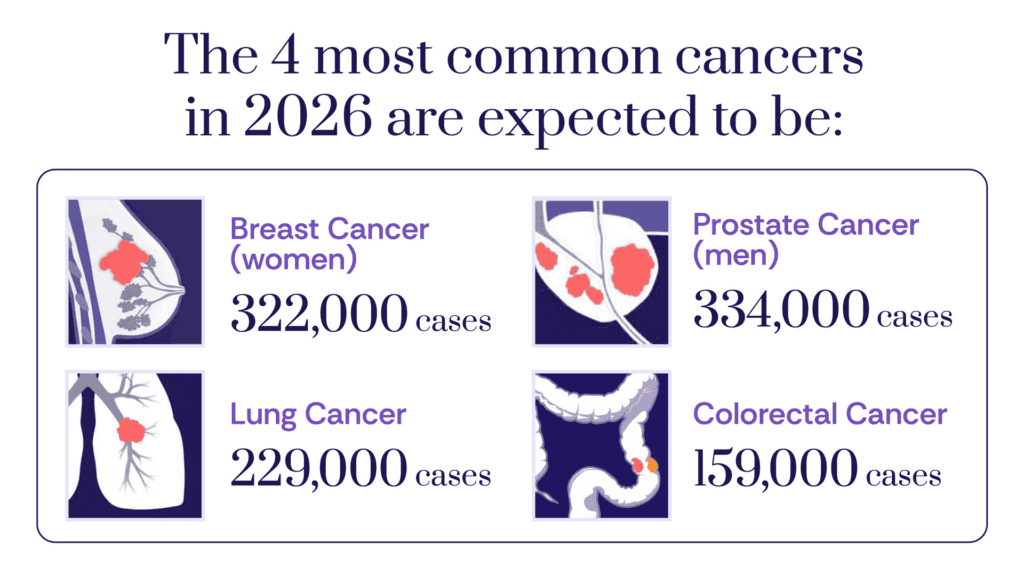
Among the various cancer types, lung cancer continues to exert the heaviest toll. The report estimates that lung cancer alone will cause more deaths than the second- and third-deadliest cancers—colorectal and pancreatic—combined. This grim statistic emphasizes the enduring legacy of tobacco use, despite significant reductions in smoking rates over the past decades, and the challenges associated with early detection and effective treatment for this aggressive disease. Colorectal cancer, while the second-deadliest, has seen some improvements in survival thanks to increased screening and advanced treatments. Pancreatic cancer, however, remains stubbornly difficult to treat, with survival rates largely stagnant, signaling an urgent need for dedicated research and novel therapeutic approaches.
Immunotherapy: Redefining the Possible in Cancer Treatment
The transformative power of immunotherapy is particularly evident in the dramatic improvements in five-year survival rates for several advanced cancers, which were once considered virtually untreatable. These are not marginal gains but fundamental shifts in prognosis. As Dr. Antoni Ribas, MD, PhD, Professor at UCLA and a member of the CRI Scientific Advisory Council, eloquently states, “When we look at metastatic melanoma survival improving from 16% to 35% in just 25 years, we’re witnessing the direct impact of immune checkpoint inhibitors like anti-PD-1 and anti-CTLA-4 therapies. These are the breakthroughs that the Cancer Research Institute has championed for decades – supporting the fundamental science that made immunotherapies a reality.” This more than doubling of the survival rate for metastatic melanoma within a quarter-century is a powerful testament to the efficacy of these novel treatments.
Beyond melanoma, immunotherapies have demonstrated significant impact in advanced non-small cell lung cancer, renal cell carcinoma, head and neck squamous cell carcinoma, bladder cancer, and Hodgkin lymphoma, among others. The mechanism involves "releasing the brakes" on the immune system, allowing T-cells to recognize and attack cancer cells more effectively. This paradigm shift from directly attacking cancer cells (as with chemotherapy) to empowering the body’s own defenses represents one of the most exciting frontiers in medicine. The durable responses observed in a subset of patients treated with immunotherapy offer long-term survival prospects that were previously unimaginable, truly rewriting the survival curves for aggressive malignancies.
Progress, Yet Uneven: Persistent Disparities and Challenges
While the overall cancer death rate has declined by an impressive 34% from 1991 to 2023, translating to an estimated 4.8 million deaths averted, the Cancer Statistics 2026 report also casts a stark light on areas where progress has been frustratingly slow and uneven. This overall decline is a multifaceted achievement, attributable to a combination of factors including significant reductions in smoking prevalence, enhanced early detection through widespread screening programs (such as mammography and colonoscopy), and, critically, the advent of improved treatments, notably the immunotherapy revolution.
However, the report underscores that the benefits of this progress are not equally distributed across all populations, highlighting persistent inequities that demand urgent attention:
Rising Cancer Rates in Young Adults: A concerning trend identified by the report is the increase in cancer incidence among young adults. While still relatively rare compared to older populations, diagnoses of certain cancers, such as colorectal cancer, pancreatic cancer, and certain breast cancers, are rising in individuals under the age of 50. This trend points to potential shifts in risk factors, including lifestyle, diet, obesity, and environmental exposures, and necessitates targeted research to understand underlying causes and develop appropriate screening and prevention strategies for this demographic. The long-term implications for public health and economic productivity are substantial.
Widening Geographic Gaps: The report reveals expanding disparities in cancer outcomes based on geographic location. Patients residing in rural or medically underserved areas often face significant barriers to accessing high-quality cancer care. These barriers include a scarcity of specialized oncologists, limited access to advanced diagnostic imaging and treatment technologies, and greater distances to treatment centers. Furthermore, regional variations in environmental exposures, lifestyle factors, and the availability of primary care services can contribute to disparities in cancer incidence and mortality. This geographic divide exacerbates existing health inequalities and underscores the need for robust initiatives to strengthen healthcare infrastructure in underserved communities, potentially leveraging telemedicine and mobile health clinics to bridge access gaps.
Persistent Racial and Ethnic Inequities Driven by Systemic Barriers: The Cancer Statistics 2026 report places a strong emphasis on the deep-seated racial and ethnic inequities that continue to plague cancer outcomes. These disparities are not merely statistical anomalies but are rooted in a complex interplay of systemic barriers. The report explicitly highlights a "higher prevalence of risk factors, medical mistrust, and lack of insurance, which hinders access to high-quality health care" as primary drivers.
- Higher prevalence of risk factors: Certain racial and ethnic groups may have a higher incidence of modifiable risk factors due to socioeconomic conditions, historical injustices, and targeted marketing of unhealthy products. For example, higher rates of obesity, diabetes, and certain environmental exposures can contribute to increased cancer risk.
- Medical mistrust: Historical abuses and ongoing experiences of discrimination within the healthcare system have fostered deep-seated mistrust among some minority communities. This mistrust can lead to delayed seeking of care, lower adherence to screening guidelines, and reluctance to participate in clinical trials, thereby impacting early diagnosis and access to innovative treatments.
- Lack of insurance: Disproportionate rates of uninsured or underinsured individuals among racial and ethnic minority groups severely limit access to preventative care, timely diagnosis, and comprehensive treatment. Without adequate insurance, the financial burden of cancer care can be catastrophic, forcing difficult choices that compromise health outcomes.
Even after accounting for factors such as stage at diagnosis and socioeconomic status, survival gaps persist. The report identifies "less access to high-quality care across the cancer continuum, from prevention to diagnosis and treatment" as the "largest contributor" to these enduring disparities. This means that even when diagnosed at a similar stage and with comparable socioeconomic backgrounds, individuals from marginalized communities often receive suboptimal care, whether it be less access to state-of-the-art screening technologies, delayed or incomplete diagnostic workups, fewer referrals to specialists, or limited access to the latest, most effective therapies, including breakthrough immunotherapies. Addressing these inequities requires a multi-pronged approach, including policy changes to expand insurance coverage, community-based interventions to build trust, culturally competent healthcare delivery, and initiatives to increase diversity within the healthcare workforce.
What the Report Means for the Future of Immunotherapy

The impressive survival gains detailed in this report are a powerful validation of decades of sustained investment in cancer immunology. However, they simultaneously serve as a stark reminder of the extensive work that remains. The immunotherapy revolution, while transformative, is still in its early stages of realizing its full potential.
- Expanding Reach: A critical future direction for immunotherapy is to extend its efficacy to a broader spectrum of cancers that currently show limited or no response. Cancers like pancreatic cancer, certain brain tumors, and many pediatric cancers remain largely resistant to current immunotherapeutic approaches. Unlocking the immune system’s power against these recalcitrant tumors requires a deeper understanding of their unique immune evasion mechanisms.
- Overcoming Resistance: Even in cancers where immunotherapy has shown success, a significant proportion of patients do not respond or eventually develop resistance. Research must focus on identifying biomarkers that predict response, understanding the mechanisms of primary and acquired resistance, and developing novel strategies to overcome these challenges. This includes exploring new immune checkpoints, targeting different immune cell types, and manipulating the tumor microenvironment.
- Combination Therapies: The future of immunotherapy likely lies in intelligent combinations. Combining immunotherapies with traditional treatments (chemotherapy, radiation), targeted therapies, or other immunotherapeutic agents holds immense promise for synergistic effects, potentially leading to higher response rates and more durable remissions.
- Personalized Immunotherapy: Tailoring immunotherapy to individual patients based on their tumor’s specific genetic mutations, immune profile, and microbiota is an emerging frontier. This precision approach aims to maximize efficacy while minimizing toxicity, moving towards truly personalized cancer care.
- Advanced Immunotherapies: Beyond checkpoint inhibitors, the field is rapidly advancing with therapies like CAR T-cell therapy, which involves genetically engineering a patient’s own T-cells to recognize and attack cancer cells. Expanding the safety and efficacy of such complex cellular therapies and making them accessible to more patients is a crucial area of development.
The Road Ahead: Sustaining Research and Ensuring Equity
The Cancer Statistics 2026 report stands as a powerful testament to the undeniable truth that research works. The immunotherapy revolution, far from an overnight phenomenon, is the culmination of decades of fundamental basic science, meticulously funded by institutions such as the National Cancer Institute and unwavering philanthropic organizations like the Cancer Research Institute (CRI). These investments have laid the groundwork for the breakthroughs that are now transforming lives.
Yet, the same data that celebrates monumental progress also starkly reveals the considerable distance we still must travel. The report highlights the stagnation of pancreatic cancer survival, which remains stubbornly low at 13%. This means that an estimated 185 Americans diagnosed with pancreatic cancer today face essentially unchanged odds compared to a generation ago, a sobering statistic that underscores a profound unmet medical need. Similarly, uterine corpus cancer mortality continues its concerning 26-year climb, demanding renewed focus on understanding its drivers and developing effective interventions. These examples are powerful reminders that while some cancers are yielding to scientific advancement, others continue to defy our best efforts.
The imperative moving forward is clear and multifaceted. Every patient, regardless of their diagnosis, deserves equitable access to the latest advances in cancer care, including breakthrough immunotherapies and targeted treatments. This necessitates not only continued research to develop new therapies but also robust health policies and infrastructure to ensure that these innovations reach those who need them most. Furthermore, every cancer type deserves the sustained research investment required for breakthroughs. The disparity in research funding and focus across different cancer types must be addressed to ensure that no patient is left behind.
Finally, and perhaps most critically, every community – irrespective of race, ethnicity, or ZIP code – deserves equal access to life-saving cancer care. The systemic barriers and inequities illuminated in the report demand urgent and comprehensive action. This includes addressing socioeconomic determinants of health, dismantling discriminatory practices within healthcare, expanding access to affordable insurance, and fostering trust in medical institutions through culturally sensitive care delivery.
The human immune system holds an extraordinary, largely untapped power to fight cancer. Continued, vigorous investment in scientific research is not just an academic pursuit; it is an ethical imperative essential to fully unlocking that power and extending its profound promise of healing and hope to patients everywhere. Only through a sustained, equitable, and collaborative effort can we aspire to a future where the burden of cancer is truly diminished for all.

