The trajectory of a young life can change in the span of a single elevator ride, a reality Jennifer, the mother of 12-year-old Isaac, understands with painful clarity. Seven years ago, Isaac was a typical five-year-old, but a series of unsettling symptoms soon replaced the sounds of the playground with the sterile hum of a hospital. Today, Isaac is a thriving middle-schooler with a passion for basketball, baseball, and football, but his journey from a high-risk leukemia diagnosis to the stage of the upcoming Glamorama event serves as a profound testament to the power of pediatric medical research and the necessity of long-term survivorship care.
The 2018 Diagnosis: A Sudden Shift in Reality
In 2018, Isaac’s family was thrust into a world of medical jargon and high-stakes decisions. What began as strange, persistent symptoms quickly escalated into a trip to the emergency department. Within hours, the family received a diagnosis that remains the primary cause of death by disease for children in the United States: leukemia. Specifically, Isaac was diagnosed with a form of the disease that would prove resistant to standard frontline interventions.
Jennifer recalls the exact moment the gravity of the situation became undeniable. It occurred on the seventh floor of the hospital, as the elevator doors opened to reveal the words "Hematology/oncology" mounted on the wall. For many families, this threshold represents the end of normalcy and the beginning of a grueling marathon. "Those doors opened, and it was like it all became real," Jennifer said, reflecting on the sight of other children undergoing treatment. "You see those words on the wall, and you see the other kids on that floor, and it all just hits you."
Leukemia, a cancer of the blood-forming tissues, including the bone marrow and the lymphatic system, accounts for nearly 28% of all cancer diagnoses in children and adolescents. While survival rates for pediatric leukemia have improved significantly over the last several decades, Isaac’s case presented unique challenges that would require more than the standard protocol.
The Limits of Conventional Treatment and the Shift to High-Risk Status
Isaac’s medical team immediately initiated high-dose chemotherapy, the traditional cornerstone of leukemia treatment. However, the expected milestone of remission—the absence of detectable cancer cells—did not materialize. When a patient does not respond to initial induction therapy, they are reclassified as "high-risk." This designation signifies a more aggressive disease profile and a statistically lower probability of long-term survival using conventional methods.
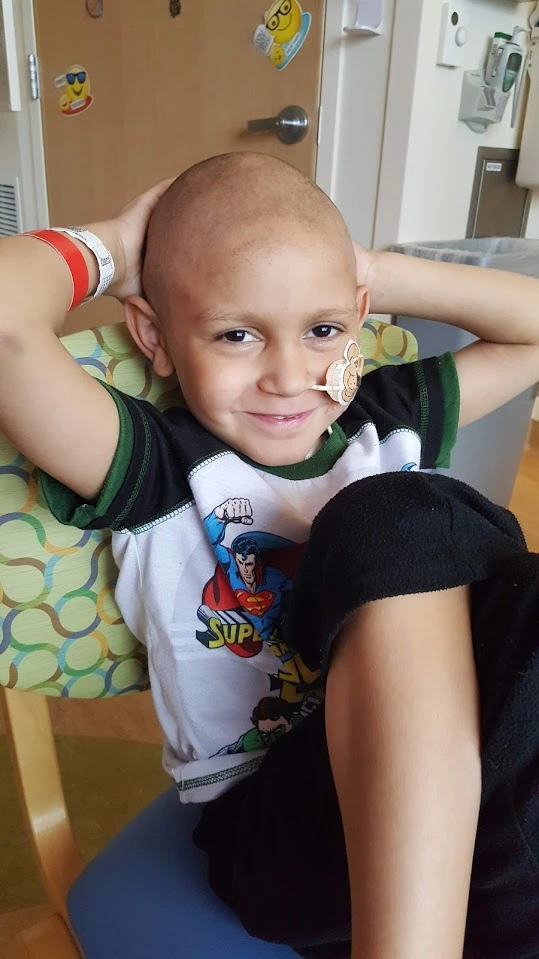
For Isaac, being a high-risk patient meant an intensification of an already grueling regimen. His life became a cycle of needle pokes, prolonged hospital isolation to protect his compromised immune system, and weeks of intravenous chemotherapy. The physical toll was compounded by severe allergic reactions to certain medications, a common but dangerous complication in pediatric oncology that further narrows the available treatment options.

As the efficacy of standard chemotherapy waned, Isaac’s prognosis grew increasingly uncertain. In the field of pediatric oncology, when traditional "off-the-shelf" treatments fail, the focus shifts toward clinical trials and experimental therapies—areas that are entirely dependent on ongoing research and philanthropic funding.
Medical Innovation as a Lifeline: The Role of Immunotherapy
The turning point in Isaac’s battle came through the application of cutting-edge medical research. Doctors proposed a relatively new form of treatment known as immunotherapy. Unlike chemotherapy, which attacks both cancerous and healthy rapidly dividing cells, immunotherapy is designed to "train" the patient’s own immune system to identify and destroy malignant cells with greater precision.
At the time of Isaac’s treatment, the specific immunotherapy protocol being considered had been approved for use in adults but had not yet been widely adapted or approved for pediatric patients. This "translational" gap—the time it takes for adult medical breakthroughs to reach children—is a significant hurdle in pediatric medicine. Because children’s bodies are still developing, medications must be carefully recalibrated for their unique physiology.
Isaac became a recipient of this adapted therapy. The results were transformative. After four rounds of immunotherapy, Isaac finally achieved the remission that chemotherapy had failed to deliver. This success paved the way for the next critical step in his recovery: a life-saving bone marrow transplant. The transplant was necessary to replace his diseased marrow with healthy stem cells, effectively resetting his blood-production system.
The University of Minnesota and the Continuum of Survivorship Care
While the successful transplant marked the end of Isaac’s active cancer, it did not mark the end of his medical journey. Modern pediatric oncology recognizes that the "cure" is only the beginning. Survivors of childhood cancer often face "late effects"—physical, cognitive, and psychological challenges that can emerge years or even decades after treatment concludes.
Today, Isaac remains under the watchful eye of the University of Minnesota’s pediatric experts. He regularly sees Dr. Karim Sadak, the Senior Medical Director of Pediatrics at the University of Minnesota and a specialist in cancer survivorship. Dr. Sadak’s role is to monitor Isaac’s holistic health, ensuring that any complications resulting from high-dose chemotherapy, radiation, or the transplant are identified and managed early.
"Survivorship care is about more than just checking for the return of cancer," medical experts at the University of Minnesota Masonic Children’s Hospital note. It involves tracking cardiovascular health, endocrine function, and cognitive development, as the intensive treatments required to save a child’s life can sometimes impact these systems. Because of this specialized follow-up care, Isaac is not just surviving; he is thriving. He has been able to return to the life of a typical 12-year-old, exploring interests in street-style fashion, learning to cook, and maintaining a busy schedule of sports and social activities.
Glamorama: A Celebration of Resilience and a Catalyst for Funding
Isaac’s journey has led him from the oncology ward to a different kind of spotlight. He is set to participate in the return of Glamorama, a high-profile event that blends fashion, music, and performance to raise awareness and funds for childhood cancer research. The event serves as a platform to celebrate the resilience of survivors like Isaac while highlighting the urgent need for continued medical innovation.
Historically, Glamorama has played a vital role in the fundraising ecosystem for the Children’s Cancer Research Fund (CCRF) and the University of Minnesota. Events of this scale are crucial because pediatric cancer research is notoriously underfunded compared to adult cancers. According to the National Cancer Institute, only about 4% of federal cancer research funding is dedicated specifically to pediatric cancers. This creates a reliance on private donations and community events to bridge the gap between discovery and life-saving treatment.
For Isaac, participating in Glamorama is an opportunity to showcase the "unstoppable" nature of children who have faced life-threatening illnesses. He will join other survivors to bring the production to life, symbolizing the creativity and courage that defined his seven-year battle.
Data and Implications: The Broader Landscape of Pediatric Oncology
Isaac’s story is a microcosm of the broader progress and remaining challenges in the field of pediatric oncology. According to data from the American Cancer Society:
- Survival Rates: The five-year survival rate for all childhood cancers has risen from less than 60% in the mid-1970s to roughly 85% today. However, for high-risk or relapsed cases, these figures remain significantly lower.
- The Cost of Cure: Up to 60% of childhood cancer survivors will experience at least one chronic health condition as a result of their treatment, and 25% will face a severe or life-threatening "late effect."
- Research Impact: The immunotherapy Isaac received is part of a burgeoning field of "targeted therapies" that aim to reduce the long-term toxicity associated with traditional chemotherapy.
The success of Isaac’s treatment highlights a critical shift in oncology toward personalized medicine. By adapting adult treatments for pediatric use and utilizing the body’s immune system, doctors are finding ways to save children who were previously considered terminal. However, the fact that Isaac’s treatment was "adapted" underscores the ongoing need for more pediatric-specific clinical trials.
Conclusion: A Living Proof of Research
The narrative of Isaac’s recovery is more than a human-interest story; it is a data point in the argument for sustained investment in medical science. Without the availability of experimental immunotherapy and the expertise of transplant specialists at a major research institution like the University of Minnesota, Isaac’s outcome might have been vastly different.
As Isaac prepares to step onto the stage for Glamorama, he carries with him the history of his 2018 diagnosis and the years of struggle that followed. He also carries the future of pediatric oncology—a future where "high-risk" no longer means "no hope," and where survivors are empowered to chase the lives they were meant to live. His journey from the seventh-floor elevator to the basketball court and the fashion runway stands as a definitive reminder that when research is funded, lives are not just saved—they are restored.

