The landscape of pediatric oncology is poised for a significant shift as CureSearch for Children’s Cancer, a leading global nonprofit, officially names Dr. John Prensner of the University of Michigan as the recipient of its 2025 Young Investigator Award. This prestigious grant is designed to catalyze high-impact research into some of the most challenging childhood malignancies, specifically focusing on Atypical Teratoid Rhabdoid Tumors (ATRT). ATRT is a rare, exceptionally aggressive form of brain cancer that predominantly affects infants and toddlers under the age of three. By targeting the "dark matter" of the human genome, Dr. Prensner’s work aims to uncover previously invisible genetic drivers that could lead to the first generation of targeted therapies for a disease that currently lacks a standard of care beyond highly toxic conventional treatments.
The Clinical Urgency of ATRT and Current Treatment Limitations
Atypical Teratoid Rhabdoid Tumor (ATRT) represents one of the most formidable challenges in modern pediatric neurology. Classified as a Grade IV tumor by the World Health Organization, it is characterized by rapid growth and a tendency to spread through the cerebrospinal fluid. These tumors typically manifest in the cerebellum or the brainstem—areas responsible for motor control, balance, and autonomic functions like breathing and heart rate. Because ATRT primarily strikes children in their first years of life, the clinical management is fraught with ethical and physiological complications.
The current therapeutic arsenal is limited to aggressive surgical resection followed by intensive chemotherapy. However, the use of craniospinal radiation—a staple in adult brain cancer treatment—is often avoided in infants due to the devastating long-term neurocognitive effects on the developing brain. Despite these grueling interventions, the prognosis remains somber, with survival rates historically hovering between 30% and 50%, depending on the molecular subtype and the extent of the tumor at diagnosis.
Dr. Paisley Myers, Director of Research and Programs at CureSearch, emphasized the disparity in treatment evolution. While adult cancers have seen a revolution in precision medicine and immunotherapy, ATRT research has lagged due to the tumor’s unique genetic profile, which often lacks the traditional mutations targeted by modern drugs. The 2025 Young Investigator Award seeks to bridge this gap by providing the financial runway for Dr. Prensner to explore non-traditional genomic pathways.
Scientific Innovation: Beyond the Traditional Genome
Dr. John Prensner’s research at the University of Michigan represents a departure from classical oncology. Most cancer research focuses on well-known genes that undergo mutations or deletions. ATRT, however, is often characterized by a "quiet" genome, frequently marked only by the loss of the SMARCB1 gene. This lack of obvious targets has left scientists in the dark for decades.
Dr. Prensner’s project focuses on small open reading frames (sORFs). Historically, these segments of DNA were dismissed as "junk DNA" or non-coding regions because they were thought to be too small to produce functional proteins. Recent advancements in ribo-sequencing and proteomics have revealed that these sORFs actually produce "microproteins"—tiny molecular machines that may hold the key to cell survival and proliferation in ATRT.
By mapping the "micro-proteome" of ATRT cells, Dr. Prensner aims to identify which of these microproteins are essential for the tumor’s growth. This approach treats the tumor’s hidden genetic landscape as a reservoir for new drug targets. If successful, the research could lead to the development of small-molecule inhibitors that specifically disable these microproteins, sparing healthy brain tissue from the "sledgehammer" effect of traditional chemotherapy.
A Strategic Partnership: The Funding Ecosystem
The 2025 Young Investigator Award is the result of a sophisticated co-funding model designed to maximize the impact of philanthropic capital. This specific grant is supported by a coalition including the Jeff Gordon Children’s Foundation (JGCF) and Violet’s Village: The Violet Kenney Legacy Fund.
The Jeff Gordon Children’s Foundation, established by the four-time NASCAR Cup Series champion, has long been a pillar in the fight against pediatric cancer. Susan Robinson, Executive Director of JGCF, noted that brain tumors remain the leading cause of cancer-related death in children. The foundation’s partnership with CureSearch is a strategic move to ensure that high-potential researchers like Dr. Prensner remain in the pediatric field rather than migrating to the more heavily funded world of adult oncology.

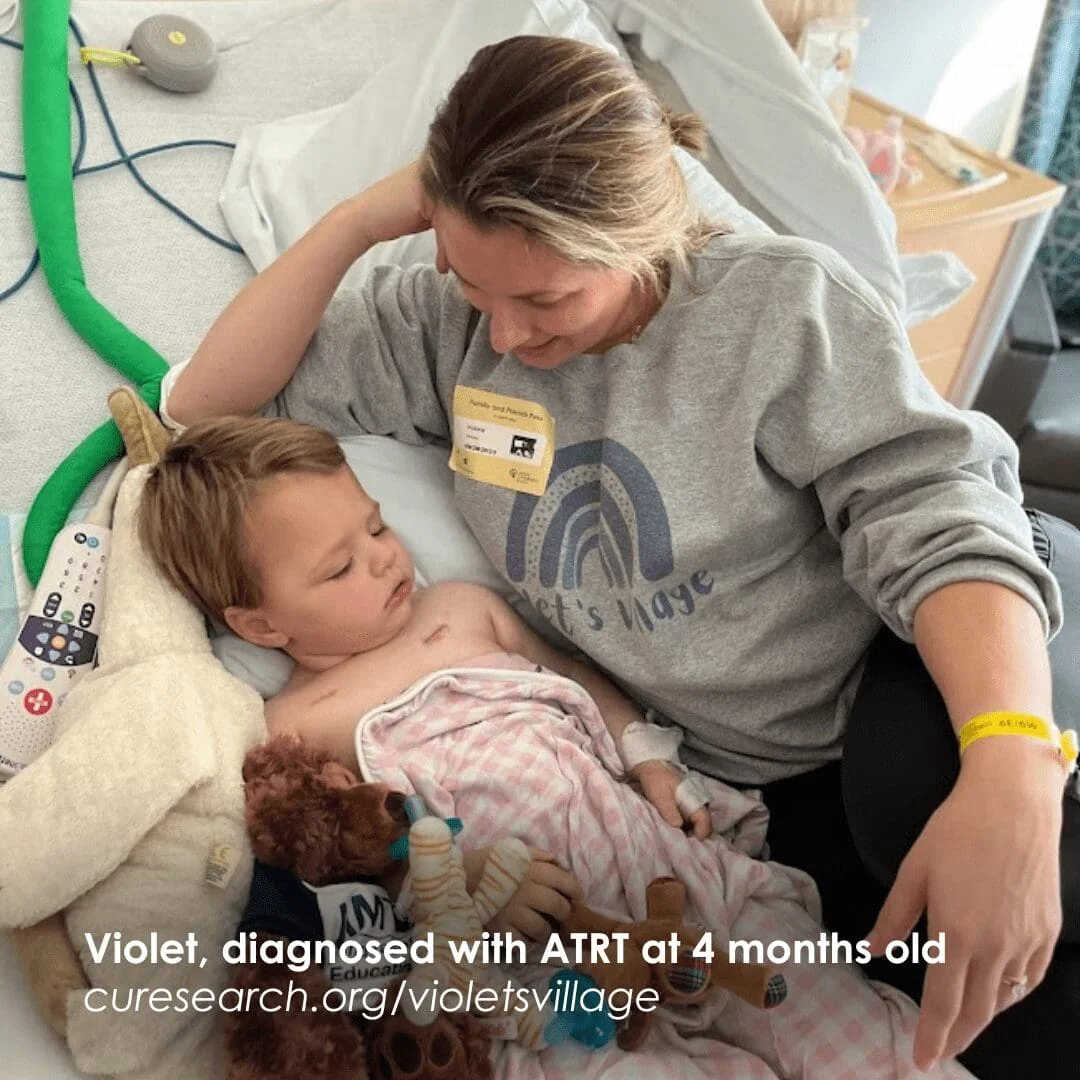
Violet’s Village represents the emotional core of this funding initiative. Named in memory of Violet Kenney, a child who battled cancer, the legacy fund at CureSearch mobilizes community-driven donations to support cutting-edge science. This collaborative approach highlights a growing trend in medical research where patient advocacy groups, celebrity foundations, and national nonprofits pool resources to tackle "orphan" diseases that receive minimal funding from federal sources like the National Cancer Institute (NCI).
Supporting Data: The Funding Gap in Pediatric Research
The necessity of the Young Investigator Award is underscored by sobering statistics regarding research funding. In the United States, the federal government allocates less than 4% of the NCI’s annual budget to pediatric cancer research. This scarcity creates what experts call the "leaky pipeline," where brilliant young scientists exit the field due to a lack of early-career stability.
Data from the American Cancer Society indicates that while the overall survival rate for childhood cancer has risen to nearly 85%, progress has been uneven. Rare tumors like ATRT have seen much slower improvements in survival compared to more common diagnoses like Acute Lymphoblastic Leukemia (ALL). Furthermore, the long-term morbidity for survivors of infant brain tumors is significantly higher than for survivors of other pediatric cancers. Chronic health conditions, including hearing loss, hormonal imbalances, and secondary malignancies, affect more than two-thirds of survivors, necessitating a desperate search for less toxic, more precise interventions.
Chronology of ATRT Discovery and Research Milestones
To understand the significance of Dr. Prensner’s work, one must look at the timeline of ATRT as a recognized clinical entity:
- 1987: ATRT is first described in medical literature, having previously been misdiagnosed as medulloblastoma or other primitive neuroectodermal tumors (PNET).
- 1998: Researchers identify the loss of the SMARCB1 (INI1) gene on chromosome 22 as the primary genetic hallmark of ATRT.
- 2010s: Genomic sequencing reveals three distinct molecular subgroups of ATRT (TYR, SHH, and MYC), each with different clinical behaviors and survival outcomes.
- 2020-2024: The focus shifts toward the "epigenetic landscape" of the tumor, as scientists realize that the way genes are turned on and off is more critical in ATRT than the mutations themselves.
- 2025: Dr. Prensner’s study of sORFs begins, marking the next frontier in understanding the tumor’s biological architecture.
Analysis of Implications for the Future of Oncology
The implications of Dr. Prensner’s research extend beyond ATRT. If sORFs and microproteins are proven to be viable therapeutic targets in one form of aggressive brain cancer, the methodology could be applied to a wide range of "cold" tumors—cancers that do not respond well to traditional immunotherapy or targeted drugs.
Furthermore, this award highlights the evolving role of the "Young Investigator." In the current scientific climate, the average age at which a researcher receives their first independent R01 grant from the NIH is over 40. By providing funding to scientists earlier in their careers, CureSearch and its partners are effectively "betting on the jockey," ensuring that the next generation of innovators has the resources to pursue high-risk, high-reward hypotheses that traditional funding bodies might overlook.
The success of this project could also influence how drug companies view rare pediatric diseases. By identifying specific, druggable targets within the sORF landscape, Dr. Prensner is providing the foundational data necessary for pharmaceutical firms to enter the space, potentially leading to clinical trials and, eventually, FDA-approved therapies specifically for toddlers with ATRT.
Conclusion and Outlook
The 2025 Young Investigator Award is more than a financial transaction; it is a critical investment in the future of pediatric medicine. As Dr. Prensner begins his work at the University of Michigan, the eyes of the oncology community—and the hopes of families affected by ATRT—are on the "junk DNA" that may finally yield a cure.
Through the combined efforts of CureSearch, the Jeff Gordon Children’s Foundation, and Violet’s Village, the fight against ATRT is moving out of the shadows. The transition from broad-spectrum chemotherapy to precision microprotein targeting represents the best hope for ensuring that a diagnosis of ATRT is no longer a terminal sentence, but a manageable condition that allows children the opportunity to grow, learn, and thrive. Progress in this field is measured not just in laboratory breakthroughs, but in the years of life returned to the world’s youngest patients.